A review of the week’s plant-based nutrition news 23rd January 2022
This week I review papers on the nutritional adequacy of plant-based diets, the impact of fibre intake on cancer outcomes, olive oil consumption and health outcomes, coffee and dementia and diet and lupus.

NUTRIENT INTAKE IN MEAT VERSUS PLANT-BASED DIETS: This is a surprisingly useful paper given that it is written by two employees of the company Unilever. The aim of the study was to assess the nutritional adequacy of meat-based diets compared to plant-based diets (mainly vegetarian and vegan). This is a systematic review of observational and intervention studies published between 2000 and January 2020 and included a total of 141 (101 studies on meat eaters, 118 vegetarians, 63 vegans) mostly from Europe, South/East Asia, and North America.
There is a lot of detail in the text, which is well worth reading. Overall, all diet patterns were found to have nutritional inadequacies. Meat-eaters were at risk of inadequate intakes of fibre, polyunsaturated fatty acids (PUFA), alpha-linolenic acid (ALA), folate, vitamin D, E, calcium and magnesium. Vegetarian and vegans had lower intakes of eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), vitamin B12, vitamin D, iron, zinc, iodine, calcium and lower levels of bone turnover markers than meat eaters. Vegans had the lowest vitamin B12, calcium and iodine intake, and also lower iodine status and lower bone mineral density. Fibre, PUFAs, folate, vitamin C, E and magnesium intakes were high in plant-based diets. Average fibre intake amongst vegans was 44g/d compared to 28g/d in vegetarians and 21g/d in meat eaters. All diet groups met protein and energy requirements. There was no mention of saturated fat intake which I assume was high in meat eaters.
The table below summarises the findings.
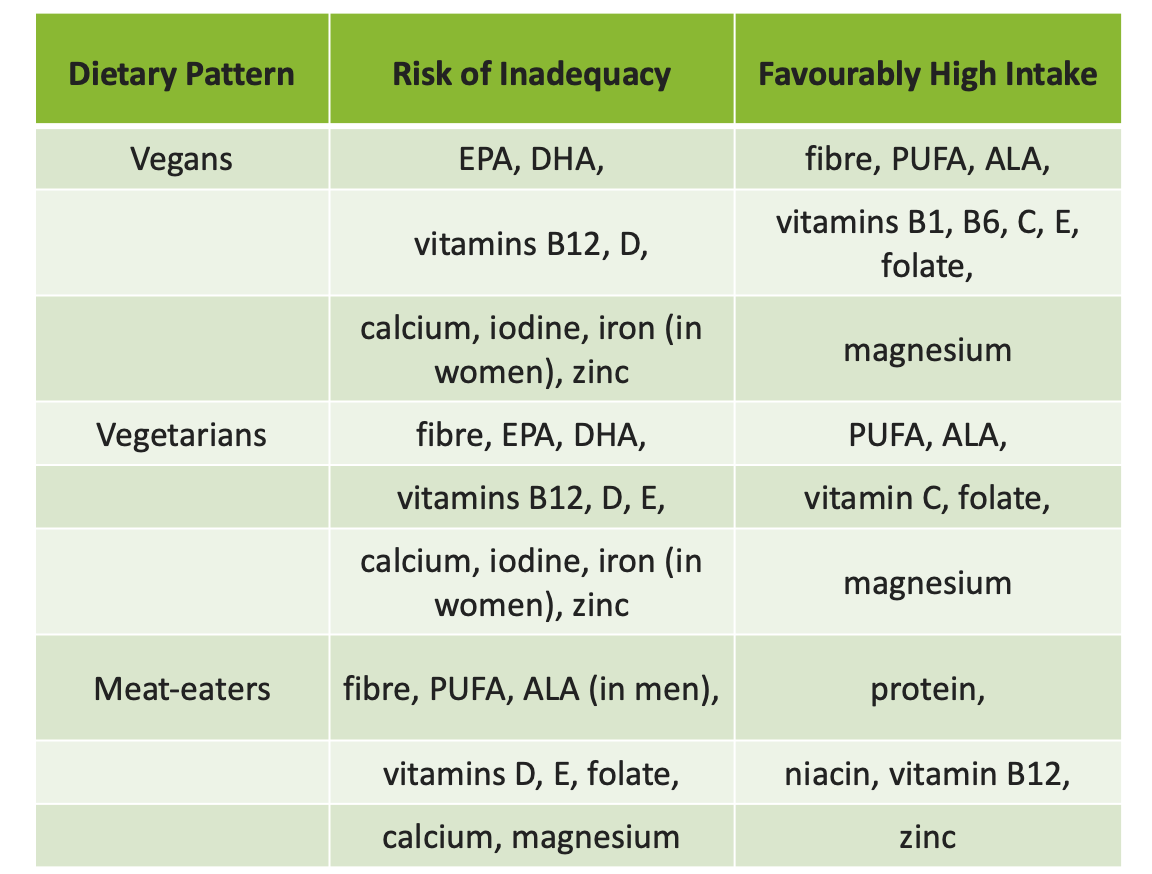
The authors’ conclusion is eminently sensible. ‘There were nutrient inadequacies across all dietary patterns, including vegan, vegetarian and meat-based diets. As plant-based diets are generally better for health and the environment, public health strategies should facilitate the transition to a balanced diet with more diverse nutrient-dense plant foods through consumer education, food fortification and possibly supplementation.’ Unilever have come out as surprising leaders in supporting a transition to a plant-based diet. Whatever their underlying motivation, they have made a valuable contribution to the literature on plant-based diets.

IMPACT OF DIETARY FIBRE ON IMMUNE THERAPY: Many of the newer cancer treatments are directed at the individuals own immune system, reactivating immune cells to enhance their ability to kill cancer cells. One of the most exciting discoveries (in my opinion) has been that the health of the gut microbiome impacts our ability to respond to these treatments. People with a healthy microbiome, with greater diversity and composed of bacteria that can produce short chain fatty acids respond better to these treatment. A fibre-rich diet is the strongest predictor of a healthy gut microbiome.
This study analysed the impact of dietary fibre and probiotic use on the gut microbiome and clinical outcomes in patients with melanoma receiving an immune activating therapy called checkpoint inhibitors. In the 128 patients included, the results showed that those consuming the most fibre (>20g per day vs <20g per day) had a better response to treatment (longer progression free survival). After adjustment for clinical factors, every 5-g increase in daily dietary fibre intake corresponded with a 30% lower risk of progression or death. Probiotic use was not associated with better treatment outcomes.
This is a really exciting observation because it suggests a safe dietary intervention could improve outcome to certain cancer therapies. This seems a much more favourable approach than faecal transplants that have been trialled to improve response in patient refractory to treatment. There may be wider implications to this research given that the gut microbiome appears to be important in outcomes from other therapies such as stem cell transplantation.

OLIVE OIL AND RISK OF DEATH: The next two studies are going to divide my followers but don’t shoot the messenger! My views are clearly stated in a previous summary article — a whole food plant-based diet can be healthy with or without added oils. Olive oil is unique amongst oils in that it has the highest ratio of monounsaturated (MUFA, mainly oleic acid) to polyunsaturated fatty acids and it contains beneficial nutrients including antioxidant phenolic compounds, vitamins, lignans, squalene and terpenoids. These compounds have been shown to have favourable biological effects in experimental models.
This paper reports results from a study that investigated the impact of olive oil consumption on the risk of all-cause and cause-specific mortality in >90,000 participants of the Nurses’ Health Study and the Health Professionals Follow-up study in the US. During the 28 years of follow up, participants who reported the highest olive oil consumption (>0.5 tablespoon/day or >7 g/d) had a 19% lower risk of all-cause mortality, 19% lower risk of cardiovascular disease mortality, 17% lower risk of cancer mortality, 29% lower risk of neurodegenerative disease mortality, and 18% lower risk of respiratory disease mortality compared with those who never or rarely consumed olive oil. This association persisted after adjustment for known risk factors and other dietary factors. As little as 1.5 g/d of olive oil was associated with a benefit in reducing mortality. The relatively novel finding is the association with reduced risk of death from dementia.
Substitution analyses found that replacement of margarine, butter, mayonnaise, and dairy fat with olive oil was associated with a reduced risk of mortality. However, substituting olive oil for other vegetable oils (eg, canola, corn, safflower, and soya bean oil) did not result in a reduced mortality risk. This suggests that other vegetable oils may provide the same health benefits as olive oil.
The authors propose that the potential mechanism for the observed benefits are a result of the high monounsaturated fat, polyphenols and other molecules such as vitamin E compounds and squalene, which together make the oil less likely to oxidise, reduce blood pressure, improve lipid profile and reduce atherosclerosis and inflammation, support the gut microbiome and improve glucose control.
The main message here is that olive oil is better than animal-derived fats. What we still need to understand is what is the amount of olive oil required for a protective effect? Is the potential effect related to MUFAs or phenolic compounds, thus confined to polyphenol-rich extra virgin olive oil and of course does olive oil add further benefits to an already healthy plant-based diet.

OLIVE OIL CONSUMPTION AND CANCER: A related study reports the impact of olive oil intake on risk of cancer. 48 studies were included in the analysis, which found that the highest olive oil consumption was associated with a 31% lower likelihood of cancer with reductions in incidence of breast, gastrointestinal, upper aero-digestive and urinary tract cancers. The positive association was only found in case-control studies rather than prospective cohort studies, which does question whether the relationship is causal. Most of the studies were in Mediterranean populations although a benefit of olive oil consumption on cancer risk was also observed in studies on non-Mediterranean populations.
The proposed mechanisms of this benefit would include the antioxidant properties of polyphenols and thus reduced DNA and cellular damage, oleic acid has been shown to favourably alter gene expression in breast cancer models and in the cells of the gastrointestinal tract.
The main limitation of the study is that there are no details of the overall quality of the diet in those consuming the most and least olive oil. We know from prior studies that the key healthy components of a Mediterranean diet pattern, which itself is associated with a lower risk of cancer, are the whole plant foods. Given that most of the studies were from the Mediterranean region this may have skewed the results. In addition, there was no analysis of dose response, the minimum amount of olive oil for benefit or information on the type of olive oil.
For me, both of these studies confirm that olive oil can be consumed as part of a healthy plant-based diet and that it is definitely a healthier source of oil/fat than animal-derived fats and oils. It may even be better than other vegetable oils. However, there is no evidence that you will adversely effect your health by not consuming oils if you are eating an otherwise healthy plant-based diet. If your health goal is to reduce and maintain a healthy body weight, then removing oil can be a beneficial and straight forward step.

COFFEE AND ALZHEIMER’S DISEASE (AD): Coffee consumption can be a healthy addition to the diet if you don’t suffer with side-effects such as palpitations, insomnia and anxiety. There are data supporting coffee consumption for reducing the risk of cardiovascular disease, type 2 diabetes and certain cancers. So could it also be protective against the develop of AD?.
As part of the Australian Imaging, Biomarkers and Lifestyle Study of ageing, researchers investigated whether self-reported coffee intake affected the rate of cognitive decline of more than 227 Australians over a ten year period. In a subset of individuals, the relationship between habitual coffee intake and cerebral A-beta-amyloid accumulation (n=60) and brain volumes (n=51) was also investigated. Deposition of abnormal A-beta-amyloid protein plaques in the brain is a key feature of AD.
The data showed that participants with higher coffee consumption at the start of the study had a lower risk of developing mild cognitive impairment, which often precedes the onset of AD. Benefits were observed in multiple domains of cognitive functioning. Higher coffee intake was also associated with slower accumulation A-beta-amyloid in the brain.
The observed effects suggest that if the average cup of coffee made at home is 240 g, increasing intake from one to two cups per day could potentially reduced the risk of cognitive decline by 8% and Ab-amyloid accumulation by 5% over an 18-month period.
The key beneficial component in coffee is yet to be established and this study did not distinguish between caffeinated and decaffeinated coffee consumption.
Although there will never be one ‘magic bullet’ to preventing AD with an overall healthy lifestyle being key, it is reassuring the one of the worlds most commonly consumed beverages may have some benefits for brain health.

PLANT-BASED DIETS AND SYSTEMIC LUPUS ERYTHEMATOSUS (SLE): We need to learn more about the impact of diet on autoimmune conditions such as SLE. There has been supportive evidence for a while that the Western-style diet pattern heavy in meat and processed foods and low in healthy plant foods has been one of the contributing factors to the rising incidence of such conditions. Many condition can improve with the adoption of a plant-based diet, including inflammatory bowel disease, multiple sclerosis and rheumatoid arthritis. There are less data supporting dietary interventions in SLE, although anecdotal yet remarkable success stories have been published. Most physicians remain reluctant to recommend intensive dietary changes and so patients are often left to experiment on their own.
This UK-based study involved administering an online survey to patients with SLE to better understand their attitudes and experiences regarding their SLE symptoms and diet.
The majority (>80%) of participants who changed their eating habits by increasing vegetable intake and/or decreasing their intake of processed food, sugar, gluten, dairy and carbohydrates reported a benefit from the dietary change with symptom severity ratings reduced by 21%. The greatest benefit in symptoms was achieved with reducing or removing dairy and processed foods and a vegan diet pattern. Common benefits included weight loss and improvements in fatigue, joint/muscle pain and mood. 57% of people who changed their diet stuck to it for over a year. Unsurprisingly, those who reported benefits stuck to the diet changes for longer and a longer duration of diet change was associated with a greater improvement in the symptoms of fatigue, joint/muscle pain, hair loss, headaches, nausea and decreasing medication use. The study also highlighted the willingness of patients to try dietary changes to improve their symptoms.
The authors conclude ‘this data suggests that increasing the quantity of plant-based foods in the diet, while decreasing processed foods and sugar, is especially beneficial for decreasing SLE symptoms long-term, especially in patients with self-perceived active lupus’.
Proposed mechanisms of these effects include weight loss and lower inflammation associated with plant-based diets along with the higher consumption of anti-oxidant compounds.
Please follow my organisation ‘plant-based health professionals UK’ on Instagram @plantbasedhealthprofessionals and facebook. You can support our work by joining as a member or making a donation via the website.
