A review of the weeks plant-based nutrition news 19th July 2020
This week it’s a win win for whole grain and fibre consumption but not a good week for animal protein!
DIET FOR ULCERATIVE COLITIS: Ulcerative colitis (UC) is an inflammatory bowel disease (IBD), along with Crohn’s disease. The cause of IBD is not fully understood but is thought to be due to a combination of genetic factors, immune dysregulation and environmental triggers. The gut microbiome play a fundamental role, with alterations in the microbiome being key for triggering chronic inflammation and the disease process. Environmental factors appear to be the key in determining whether someone with a genetic predisposition develops the illness and these factors include diet, smoking, alcohol and drugs/medications. The key components of the diet that are implicated in the pathogenesis are diets high in saturated fat and sugar and low in fibre. Food additives, including emulsifiers (carboxymethylcellulose and polysorbate-80), maltodextrin (used as thickeners and sweeteners) and carrageenans, used for texture and as thickening agents in the dairy and sauce industry, are also implicated.
The use of plant-based diet in IBD has been pioneered by Japanese researchers who have been using this in clinical practice for over 15 years, with remarkable results. Their plant-based diet is really a semi-vegetarian diet that includes yogurt and allows for fish once a week to make it more acceptable to patients. Their plant based diet scoring system considers eight foods to be preventive factors for IBD (vegetables, fruits, pulses, potatoes, rice, miso soup, green tea, and plain yogurt) and eight foods to be harmful (meat, minced or processed meat, cheese/butter/margarine, sweets, soft drinks, alcohol, bread, and fish). They have acheived very good results and durable remissions in both UC and Crohn’s and have also demonstrated higher remission rates in combination with biologic therapies. They have not found a negative impact with the high fibre content despite the prevailing advice to limit fibre consumption in the acute phase of the disease.
The 2020 guidance from the International Organisation for the Study of IBD is summarised below. The trouble with diet data is that it is generally of low to moderate quality due to the inate issues with conducting studies of diet and health.

Getting back to the study highlighted, it reports the results of 17 patients with UC who took part in a cross-over trial of a low-fat, high fibre diet versus an improved version of the standard American diet (SAD; with increased fruit, vegetables and fibre). These participants were in remission or had mildly active disease and 15 of 17 were on active treatment. Participants were randomly assigned to 2 groups and received a low fat high fibre diet (10% of calories from fat) or an improved SAD (35%–40% of calories from fat) for the first 4-week period, followed by a 2-week wash-out period, and then switched to the other diet for 4 weeks. All diets were catered and delivered to patients’ homes. The main study outcome was quality of life but serum inflammatory markers were measured and stool testing for changes in the gut microbiome was also performed.
The results showed that the baseline diet of the participants was pretty unhealthy, being low in fruits and vegetables and high in refined sugar with a median of 12g of fibre consumed per day. Thus both interventions improved diet quality and resulted in improvements in indicators of quality of life. But the low fat, high fibre diet led to more significant reduction in serum markers of inflammation and more favourable changes in the gut microbiome. Both diets were higher in fibre than the participants baseline diet with a median of 18g/day in the improved SAD and 26g/day in the low fat high fibre diet but they were well tolerated without exacerbation of symptoms. The low fat, high fibre diet was higher in fruits and vegetables and lower in red meat, resulting in increased consumption of micronutrients and lower consumption of saturated fat and cholesterol.
This is a small study and needs to be replicated, but it does highlight the possibility for diet interventions in UC with no detrimental effects of increased fibre consumption in patients in clinical remission or mildly active disease.
WHOLE GRAIN CONSUMPTION REDUCES THE RISK OF TYPE 2 DIABETES: This paper was in the same issue of the BMJ as the paper I covered last week demonstrating that increased consumption of fruits and vegetables is protective against type 2 diabetes. This study reports results from the Nurses’ Health Study and the Health Professionals follow-up study from the US and included 158 259 women and 36 525 men who did not have type 2 diabetes, cardiovascular disease, or cancer at baseline. During the average follow up of 24 years, 18 629 participants developed type 2 diabetes.
Total whole grain intake was categorized into five equal groups; never or less than one serving a month; one serving a month to one serving a week; and two or more servings a week. For whole grain cold breakfast cereal, dark bread, and popcorn, four categories were used because these foods had relatively higher overall intake; never or less than one serving a month; one serving a month to one serving a week; one serving a week to 4–6 servings a week; and one or more servings a day.
After adjusting for other lifestyle factors and dietary components, those consuming the highest amount of whole grains, compared to the lowest, had a 29% reduction in the risk of developing type 2 diabetes. When examining the consumption of individual foods, whole grain cereal, oatmeal, brown rice, wheat germ and dark bread all resulted in a significantly lower risk of type 2 diabetes with risk reductions in the order of 15–20%. It should be noted that there was an increased risk of type 2 diabetes in those consuming more than one portion of popcorn per day. This finding warrants further investigation and may be due to the fact that popcorn consumption is often associated with toppings of salt, fat and sugar.
Whole grains are a rich source of fibre, antioxidants, B vitamins, magnesium, phenols, phytooetrogens and other phytochemicals. Studies have shown that whole grain consumption is associated with reduced fat mass, increased insulin sensitivity, improved lipid profile and reduced inflammation. Taken together with the results of other studies and the companion paper from last week, it seems clear that consumption of fruits, vegetables and whole grains provides significant protection against type 2 diabetes. When you add in the known beneficial effects of beans and legumes for diabetes prevention, you have the basic components of a whole food plant based diet. No other foods have so consistently been shown to be beneficial. These data should be informing public policy and country based dietary guidelines.
WHOLE GRAIN AND FIBRE CONSUMPTION REDUCES THE RISK OF COLORECTAL CANCER: The WHO and the World Cancer Research Fund have concluded that the consumption of fibre and whole grains significantly reduces the risk of colorectal cancer (CRC). Dietary fibre acts by increasing stool bulk, thus diluting potentially carcinogenic substances, decreasing transit time through the bowel, and promoting fermentation and short chain fatty acid production in the gut. However, results from studies that isolate fibre from whole foods have been inconsistent, and it has been unclear to date whether the benefits of fibre are due to the nutrient itself or from the whole foods that naturally contain it.
This study analysed data from the NIH-AARP Diet and Health Study, which included 478,994 participants aged 50–71 years at baseline and followed for more than 15 years, with 10,200 incident cases of CRC. It represents the largest cohort analysis to date of the association of whole grain and dietary fibre intake with CRC risk. The study showed that whole grains and fibre from grains, but not total dietary fibre consumption, was inversely associated with CRC risk. Compared with those in the lowest quintile (0.1 servings per 1000kcal per day) of intake of whole grains, those in the highest quintile (1.3 servings per 1000kcal per day) of intake of whole grains had a 16% lower risk of CRC, with an even greater risk reduction of 24% for rectal cancer.
This study confirms the value of concentrating on the consumption of whole foods rather than focusing on individual nutrients. Fibre consumption is key to maintaining health but foods such as whole grain that contain fibre come packaged with so much more and its the entire package that is beneficial to health.
WHICH SOURCE OF PROTEIN IS BEST — ANIMAL OR PLANT: Recurrent media stories try and convince us that animal sources of protein are best and of higher quality. Protein quality should not be judged on whether it contains all the amino acids and how digestible they are, but on the impact of the protein source on health outcomes. Yet another study this week confirms improved health outcomes when animal protein is replaced by plant protein
The study highlighted from this weeks JAMA again reports data from the NIH-AARP Diet and Health Study in the US, including more than 400,000 men and women aged 50–71 years at enrollment in 1996 and observed for 16 years.
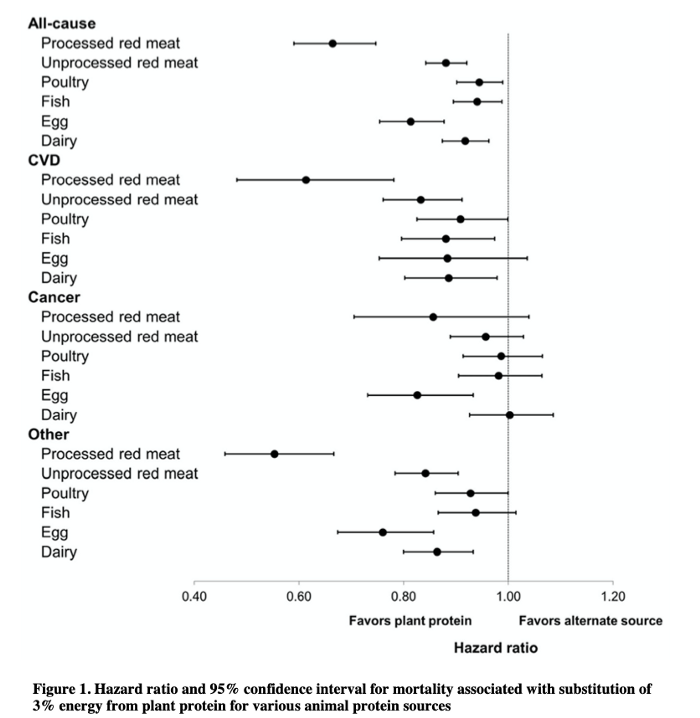
The results clearly showed that a higher intake of plant protein was associated with a significantly reduced risk of death from all causes and cardiovascular disease. For every 10g/1000kcal intake of plant protein, there was a 12–14% reduced risk of death. Replacing just 3% animal protein with plant protein reduced death by around 10% and replacing both egg and red meat with plant protein was shown to be beneficial.
Why is animal protein harmful? It creates oxidative stress and inflammation; it comes packaged with saturated fat; there is higher exposure to haem iron and AGE’s, which are harmful; it contributes to adverse effects on the gut microbiome and the production of higher levels of TMAO (implicated in atherosclerosis); increased levels of growth hormone such as insulin-like growth factor, implicated in cancer risk; higher consumption of branched chain & sulphur containing amino acids, which have negative health effects.
This it not the first study to show these finding with similar results from the Nurse’s Health Study and Health Professionals follow up study, Adventist Health Study, Japanese and Finnish cohorts and the Netherlands. The image below is taken from the Nurses Health Study and Health Professionals F/U study and shows that swapping out any source of animal protein, including fish, eggs and dairy, for plant sources of protein is beneficial for health outcomes.
When considering food and nutrients, the entirety of the data needs to be considered from observational, mechanistic and interventional studies. All therapeutic diets including the DASH, Mediterranean, vegetarian and whole food plant based, minimize animal protein and emphasize plant foods with significant improvements in health outcomes. In the absence of malnutrition, no long term study has shown a benefit to increasing protein from animal sources. Don’t fall for media hype. The science is clear. Focus your diet on healthy plant foods. Western societies have a crisis of fibre and phytonutrient deficiency not protein deficiency and in fact we are suffering the consequences of protein excess.

SWAPPING OUT ANIMAL PROTEIN FOR PLANT PROTEIN PROTECTS HEART FUNCTION LATER IN LIFE: In case I didn’t convince you with the study above, this study examines the impact of protein consumption on heart function. The data are from the Bogalusa heart study and includes 456 black and white men and women with a median age of 36 years at baseline and followed for 13 years. The study examined diet intake and assessed heart function by echocardiogram. It studied left ventricular diastolic dysfunction (LVDD), an early sign of heart failure that is potentially reversible.
The mean protein consumption of the participants was 74g/day. The mean of the lowest tertile was 45.5g/day and that of the highest (wait for it!) was a wapping 107g/day. The mean range of animal protein per day was 30–75g/day. When you compare this to the generous recommendations of 0.8g/kg lean body weight, these are crazy high levels for the general population. The results showed that those consuming the most protein compared to the least had a 3x increased risk of developing LVDD. Those eating the most animal protein had at least a 2x increased risk of LVDD. Those eating the most vegetables and legumes had at least a 50% reduced risk. Swapping red/processed meat and eggs for vegetables and legumes significantly reduced the risk of LVDD. The risk of LVDD was higher in black compared to white participants.
This is not the first study that has shown a protective effect of plant protein in heart function and the good news is that early stages of heart failure may be reversible if the heart cells are allowed to heal and damaging toxins are removed. As Dr Chidi Ngwaba said in his webinar last week; The main question you have to ask of your diet choice is ‘does it keep my heart healthy?’ If it doesn’t, then it’s not worth the risk. People often forget that heart failure has just as bad a prognosis as many cancers and greatly reduces quality of life.
Here is an excellent review of diet and heart failure from plant-based dietitian Dr Conor Kerley. The images below are taken from the paper.


DO YOU NEED ANIMAL PROTEIN TO BE MASCULINE? The prevailing narrative continues to suggest that in order for men to be masculine and a ‘real man’, they needs to eat meat. This paper completely trashes that narrative. The study examines the association between a plant-based diet and serum testosterone levels in men from the national health and nutrition examination survey (NHANES) database in the US. Using the food frequency questionnaire, dietary intake was assessed using the plant-based diets index as described here. The overall plant-based diet index (PDI) and a healthful plant-based diet index (hPDI) was used with a higher score on PDI and hPDI indicating a higher consumption of plant foods. 191 male participants were included with an average age of 45 years. The results showed the expected inverse relationship between higher BMI and age and testosterone levels. However, the plant-based food content of the diet had no impact on testosterone levels. So that’s another myth cleared up. A healthy plant-based diet can make you more manly because men are less likely to suffer erectile dysfunction, which is actually one of the first signs of heart disease. The arteries in the penis are affected by atheraosclerosis in the same way as the arteries surrounding the heart. Because of their small size, symptoms of erectile dysfunction occur earlier than those of heart disease. Medication used to treat heart disease can also have side effects of erectile dysfunction. So ditch the meat and load up on plants and you can for sure be as manly as you want.
If you have found this article useful, please follow my organisation ‘plant-based health professionals UK’ on Instagram @plantbasedhealthprofessionals and facebook. You can support our work by joining as a member or making a donation via the website.