A review of the week’s plant-based nutrition news 1st March 2020
So many nutrition studies in the last few weeks, its hard to pick the best! Here are my top picks.
TMAO LEVELS PREDICT FOR CORONARY HEART DISEASE. PLANT-BASED DIETS LOWER THIS RISK: A simple conclusion from a well conducted study. 760 women from the Nurses’ Health Study were followed for 14 years. Blood samples were taken at baseline and after 10 years. Those with the highest level of TMAO (trimethylamine oxide) had a greater risk of coronary heart disease. There was also a strong correlation with increasing levels over the 10 year period and inverse association with decreasing levels — so you can change your risk over time. There was a 58–79% higher risk of developing coronary heart disease compared to those with the lowest TMAO levels.
The lowest levels of TMAO were associated with plant-based eating patterns as assessed by the Alternate Healthy Eating Index and the plant-based diet index.
So what is TMAO and what can we do about it? It is produced from gut bacteria that convert choline and carnitine from eggs and meat to TMA. Once in the bloodstream, TMA is converted to TMAO in the liver. High levels of TMAO not only increase the risk of coronary heart disease but also heart failure, renal failure and type 2 diabetes.
There is good news here. Removing red meat from the diet can bring down TMAO levels within a few weeks. Vegan and vegetarian diets are associated with lower levels of TMAO than omnivorous diet patterns. So you can alter your risk of chronic disease very easily without medications and stents but with diet change. Act now, as this study shows it’s never too late.
ANIMAL VS PLANT PROTEIN — WHICH IS BEST FOR HEALTH? This large study answers the question very clearly. Data are derived from a population-based cohort in the Netherlands (7768 participants followed for 13 years) and confirmed in a meta-analysis of 11 prospective cohort studies (350,452 participants).
Protein from meat and dairy was associated with significantly higher risk of all cause mortality and cardiovascular disease (CVD) mortality. On the other hand, plant-derived protein from fruits, vegetables, nuts and legumes, was associated with lower all-cause and CVD mortality.
What are the potential mechanisms for this negative effect of animal protein? 1) the amino acids including higher amounts of branched chain & aromatic amino acids that are associated with insulin resistance and higher body weight 2) saturated fat and salt that accompanies animal protein, which are linked to higher risk of CVD.
This study brings together a large body of evidence supporting the consumption of plant protein in preference to animal-derived protein. Negative effects on health were evident for meat AND dairy protein but not for fish or egg protein. Regarding eggs in the Rotterdam study, there was not a big difference in consumption between groups, which may have impacted on results. Other studies have shown a negative impact of egg consumption on CVD risk and mortality. Plant protein comes packaged with fibre, phytonutrients and healthy fats which promote health.
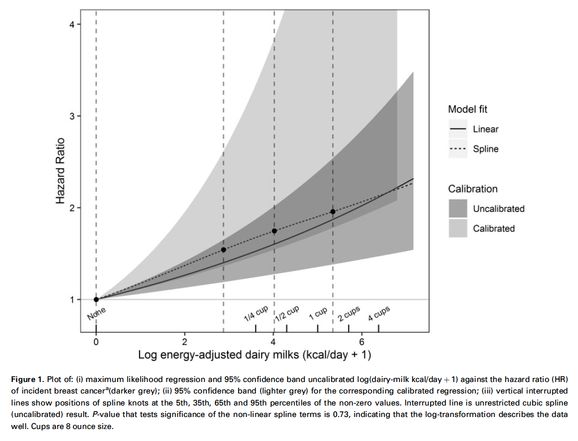
DAIRY MILK INCREASES THE RISK OF BREAST CANCER — DATA FROM THE ADVENTIST HEALTH STUDY 2: The data on dairy milk consumption and breast cancer risk is mixed. Given the high levels of oestrogen and growth hormones, it has always been hypothesized that consumption could drive breast cancer. This new study uses data from the Adventist Health Study 2 from North America. It’s note worthy that just over a quarter of participants are black. The Adventists follow 4 main diet patterns — omnivore, pescatarian, lacto-ovo vegetarian and vegan. They are also healthier than the general US population as they are physically active and mostly avoid smoking, alcohol and caffeine.
This study included >50,000 women, median age 57, followed for 8 years. 1057 cases of breast cancer were identified. The data showed that those drinking the most milk and obtaining the most calories from dairy had a significantly higher risk of developing breast cancer. Risk increased in the order of 20–50%. The association was non-linear with the greatest risk occurring at low levels of consumption (90–100 calories per day or 150mls whole milk). Soya consumption per se did not affect breast cancer risk. However, in substitution analysis, those consuming soya milk rather than dairy had a 32% reduced risk of developing breast cancer.
How might dairy milk increase risk of breast cancer? Possible mechanisms include the presence of growth factors such as oestrogen and IGF-1. Casein, the main protein in milk, at least in the lab, accelerates cancer growth. The presence of bovine leukaemia virus in US dairy cows could be implicated as this virus has been found in breast tissue.
Soya milk contains isoflavones that block endogenous oestrogen, reduce cell proliferation and help repair DNA.
This is not a perfect study. Diet was only measured at baseline and there may be residual confounding. Nonetheless, the take home message is that soya consumption does not drive cancer growth and there is a chance that swapping cow’s milk for soya in women could significantly reduce the risk of breast cancer. Don’t forget that we already know that dairy consumption significantly increases the risk of prostate cancer. Looks like dairy is a no no for men and women !
FOOD, NUTRIENTS AND BREAST CANCER RISK: Sticking to the topic of breast cancer, this study examined the association between intake of 92 foods and nutrients and breast cancer risk. The data are from 272,098 women participating in the European Prospective Investigation into Cancer and Nutrition (EPIC) study and there were 10, 979 cases of breast cancer. Six foods and nutrients were found to be associated with the risk of breast cancer. Higher consumption of total alcohol, beer/cider and wine significantly increased the risk of breast cancer, whereas higher consumption of fibre, apple/pear and carbohydrates reduced the risk. These findings were only apparent for post-menopausal and not pre-menopausal breast cancer.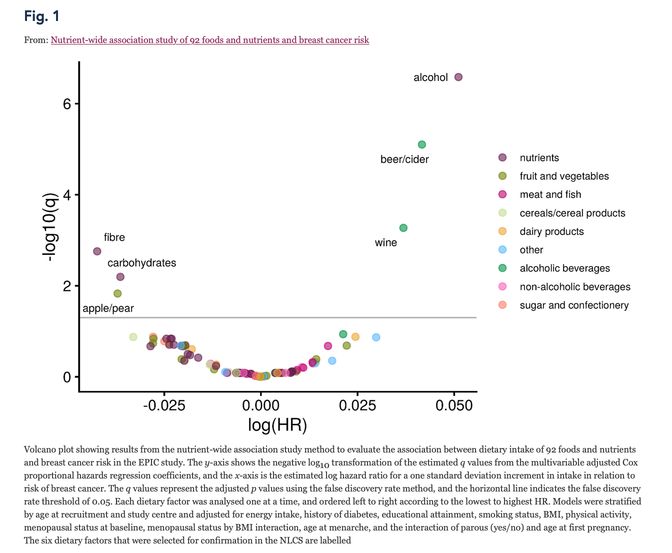
It is interesting that in this study dairy consumption did not impact the risk of breast cancer. It must be noted though that this study would not have analysed no dairy vs some dairy and soya was not one of the 92 nutrients/food analysed.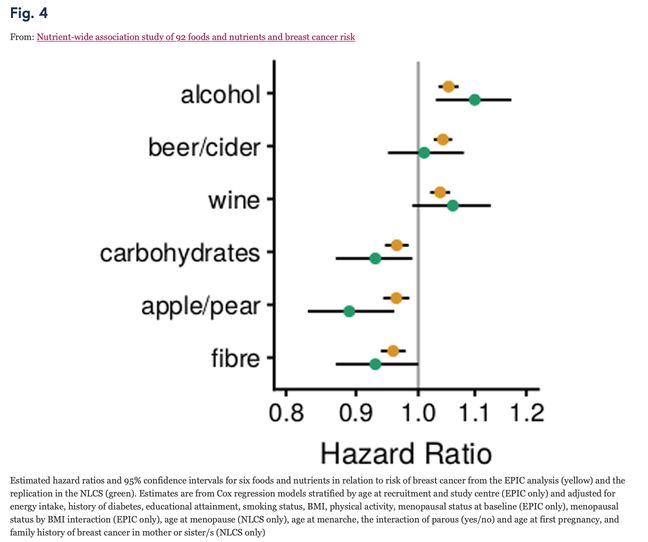
Studies of diet and breast cancer have general been inconsistent. However, the link between alcohol and increased risk is pretty solid, as is the link between fibre consumption and reduced risk. What is less consistent in the literature is the type and source of fibre. This seems less important since the basis of a healthy diet is to eat a wide range of whole plant foods. The association of dietary fat and breast cancer risk has also generated inconsistent results. However, the data does support limiting saturated fat intake in order to improve outcomes after a diagnosis of breast cancer. A meta-analysis of 15 cohort studies reported that saturated fat consumption negatively impacts breast cancer survival. In a recent report from the Women’s Health Initiative study showed that those on a lower fat diet with increased consumption of fruits, vegetables and whole grains had improved survival after a diagnosis of breast cancer.
DIET AND MENTAL HEALTH AND WELL-BEING: Mental health disorders are a significant burden of disease globally, with 1 in 4 people receiving a diagnosis in their lifetime. Several factors contribute to these disorders and diet and nutrition is one. It is clear from randomised studies such as the SMILES study and the HELFIMED study that diet interventions have a positive impact on mood disorders, with the Mediterranean diet being studied most extensively.
This systematic review analyzed the association between the intake of fruit and/or vegetable and mental health in adults. 61 studies were included. The studies included mainly focused on depression and depressive symptoms, but also other characteristics ranging from general and mental well-being, quality of life, sleep quality, life satisfaction, flourishing, mood, self-efficacy, curiosity, creativity, optimism, self-esteem, stress, nervousness, or happiness, to anxiety, minor psychiatric disorders, distress, or attempted suicide, were analyzed. The results indicated that high total intake of fruits and vegetables, and some of their specific subgroups including berries, citrus, and green leafy vegetables, may promote higher levels of optimism and self-efficacy, as well as reduce the level of psychological distress, ambiguity, and cancer fatalism, and protect against depressive symptoms. However, as with every systematic review the studies included were conducted using various methodologies and in different populations, so their results were not always comparable.The vast majority of the included studies indicated that the intake of fruits and/or vegetables and their specific subgroups, as well as processed fruits and vegetables, have a positive influence on mental health.
SALT CONSUMPTION — AN ISSUE FOR ALL DIET PATTERNS: Salt in the diet is mainly from processed and packages meals and those eaten outside the home (restaurants!). With the rise of vegan processed foods, it’s a problem for all diet patterns. In the UK, more than half of food bought by households is ultra-processed. High blood pressure is the 4th highest risk factor for death and disability in the UK and affects 1 in 4 adults. Reducing salt consumption is known to have a beneficial effect on blood pressure. The paper highlighted examines the impact of salt reduction on blood pressure and reports a large meta-analysis and systematic review of 133 studies with 12,197 participants. The results show that sodium reduction leads to a significant reduction in systolic blood pressure in adults, both female and male, all ethnic groups, and in both hypertensive and normotensive populations. Diastolic blood pressure also decreased significantly. There was a dose-response relationship with a greater reduction in sodium intake producing a greater fall in blood pressure. Populations with older age and higher baseline blood pressure achieved greater blood pressure lowering from the same amount of sodium reduction and so did non-white compared with white populations.
We already know that vegetarian diets can reduce blood pressure. Eating less salt and a plant-strong diet (DASH diet), blood pressure can be reduced by 21 points systolic and 8 points diastolic. This is like going from 150/90 to 129/82. This is way more than the effect of a blood pressure lowering medication. Did you know that the FDA requirement for new blood pressure lowering medication is that it lowers BP by around 4mmHg ?!!
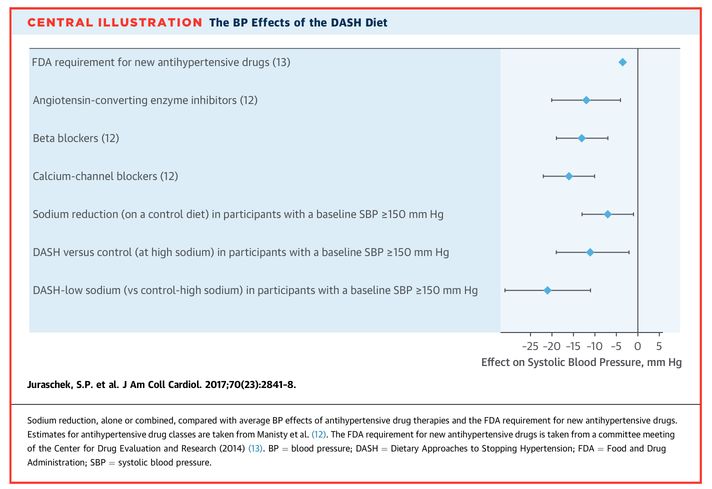
To maintain a healthy blood pressure it is probably best to remove added salt from the diet. The WHO recommends that adults consume less than 5g (just under a teaspoon) of salt per day and for children that the recommended maximum intake of salt for adults be adjusted downward for children aged two to 15 years based on their energy requirements relative to those of adults.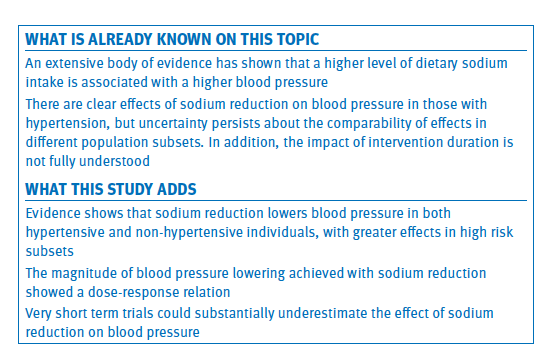
If you have found this article useful, please follow my organisation ‘plant-based health professionals UK’ on Instagram @plantbasedhealthprofessionals and facebook. You can support our work by joining as a member or making a donation via the website