This week we have had some media coverage in our support of the No Meat May campaign, highlighting the wider impact of meat consumption on human health.

The science supporting plant-based diet continues to accumulate. Here are my highlights.

DIET AND CARDIOVASCULAR DISEASE: Cardiovascular disease (CVD) remains the top cause of death globally, with unhealthy diets being the main risk factor. The strongest evidence supporting a predominately plant-based diet is for the prevention of CVD, particularly coronary heart disease. This study is a comprehensive review of dietary patterns and specific foods and nutrients on the risk of CVD. The study includes 54 systematic reviews with meta-analyses (SRMA), including 35 SRMAs of observational studies, 10 SRMAs of RCTs, and 9 SRMAs of combined RCT and observational studies.
SPOILER ALERT: COFFEE AND CHOCOLATE CONSUMPTION IS HEART HEALTHY!
The main headline findings include the following;
- A healthy diet, such as the Mediterranean, DASH and vegetarian diets can provide up to 50% reduction in risk of CVD (both coronary heart disease and stroke) and death from CVD.
- Common characteristics of healthy diet patterns include a lower intake of red and processed meats, refined carbohydrates, sugar-sweetened beverages, and whole-fat dairy products; a higher consumption of fruits, vegetables, whole grains, nuts, and legumes.
- A high intake of whole grains, legumes, fish, chocolate, and drinking one cup of coffee per day significantly decreases the risk of CVD mortality.
- A high intake of legumes, nuts, and chocolate, as well as a vegetarian diet reduces the risk of coronary heart disease.
- High intakes of vegetables and fruits, extra-virgin olive oil, and nuts, as well as dinking 1–3 cups of green tea per day significantly lowers the risk of stroke.
- High dietary fibre intake lowers both CVD risk and mortality.

My take home messages
- Concentrate on an overall healthy diet pattern rather than fixating on particular foods and nutrients.
- The more the diet is centred around whole plant foods the better for cardiovascular health.
- Fish is certainly better than eating meat but it is unlikely to be required for optimal cardiovascular health. More studies that compare the Mediterranean diet with fish to a whole food plant-based diet without fish are needed.
- Extra-virgin olive oil can be a healthy component of the diet but is not essential.

DIET AND INFLAMMATORY BOWEL DISEASE: Inflammatory bowel disease (IBD — Crohn’s and Ulcerative Colitis) is on the rise. The cause is a combination of genetic risk together with dietary and environmental factors. It is becoming clear that the risk of IBD can be significantly reduced by adopting a healthy plant-based diet pattern. Even if you have a diagnosis of IBD, the disease can be controlled and in some cases reversed by a plant-based diet intervention.
This study from the US examines data from the cross-sectional National Health Interview Survey. It compared various dietary and lifestyle factors in people with and without IBD. The IBD population was found to drink less 100% fruit juice and eat more cheese and cookies than the non-IBD population. Consumption of fries, sports and energy drinks and more frequent drinking of regular soda were significantly associated with the likelihood of having IBD. Popcorn and milk consumption were associated with a lower risk. Foods typically labeled as junk food were positively associated with a diagnosis of IBD.
This is not the best study because the design can not prove cause and effect. However, but the data are consistent with the results of more robust prospective cohort studies. The key components of the diet that are implicated in the pathogenesis are diets high in saturated fat and sugar and low in fibre. Food additives, including emulsifiers (carboxymethylcellulose and polysorbate-80), maltodextrin (used as thickeners and sweeteners) and carrageenans, used for texture and as thickening agents in the dairy and sauce industry, are also implicated. These adverse dietary factors alter the gut microbiome in an unfavourable way, leading to overgrowth of pathogenic bacteria, reduced bacterial diversity, inflammation and increased intestinal permeability. There has been recent publication of international consensus on diet and IBD, which you can find here.

DIET AND NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD): NAFLD is on the rise and is now the second commonest reason for liver transplantation in the UK. The key drivers of NAFLD are obesity, dyslipidaemia, insulin resistance and metabolic syndrome. These factors are intimately related to diet and lifestyle. In general, diets high in animal foods, saturated fat and refined grains and sugars are associated with a higher risk of developing NALFD. Lifestyle interventions are the mainstay of first-line treatment.
This study included 963 participants with a median age of 71 years and a mean BMI of 27 from the Rotterdam Study. 343 participants had NAFLD. Follow-up data was available for 737 participants at a median of 4.4 years. Diet data was analysed and grouped into patterns as shown in the heat map below. The liver was assessed by ultrasound and FibroScan, to assess liver stiffness (a sign of fibrosis).
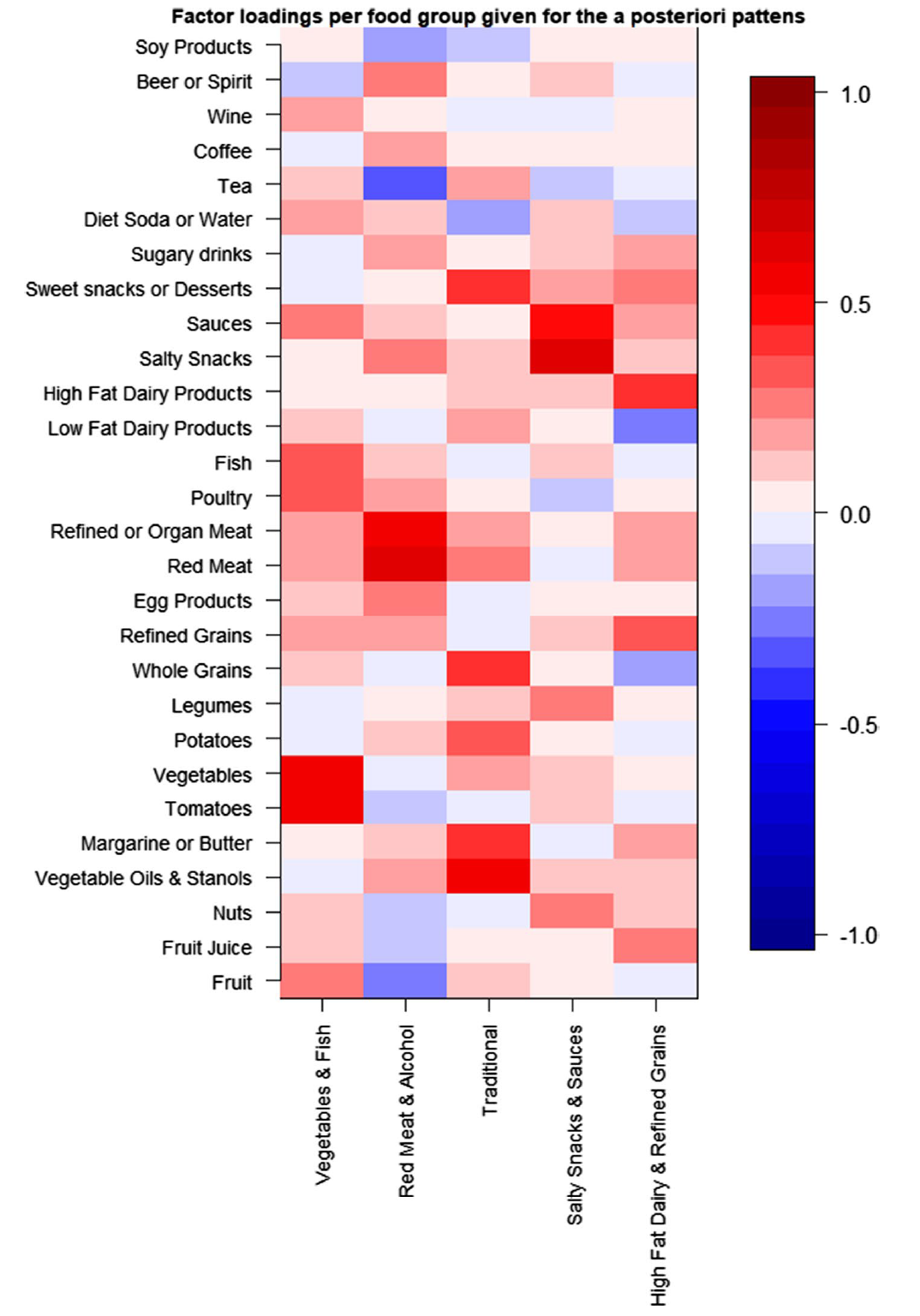
The results showed that diet patterns characterised as plant-based, high-fibre and low-fat were associated with regression of NAFLD over time. This finding is in line with increasing evidence that animal-based diets are negatively associated with NAFLD and other metabolic comorbidities.

DIET AND COGNITIVE FUNCTION: I have recently highlighted two papers that support higher intake of flavonoids from plant-based foods for prevention of cognitive decline and dementia. This study examines the impact of the consumption of another phytonutrient— carotenoids — on cognitive function. Carotenoids are a group of naturally occurring pigment compounds found in red, yellow, orange, and dark green fruits and vegetables. Beta carotene, alpha carotene, and beta cryptoxanthin are precursors of vitamin A, which is not otherwise found in whole plant foods.
This study reports data from the Nurses Health Study and includes 49,493 women with a mean age of 48 years at baseline in 1984. In 2012–2014, 41% had good cognitive function, 47% had moderate function, and 12% had poor function. Long-term higher intake of total carotenoids (median intake of 21.7 compared with 9.40 mg/d) was associated with 14% lower odds of moderate cognitive function and 33% lower odds of poor cognitive function in later life, after extensive adjustment for dietary and non-dietary variables. Similar associations were observed for each individual carotenoid, including β-cryptoxanthin, lycopene, β-carotene, lutein + zeaxanthin, and α-carotene. The hypothesis for this finding is that carotenoids reduce oxidative stress and hence inflammation, thus protecting brain function.
In general, it is not helpful to concentrate on individual nutrients, but the accumulating data supports the benefits of fruits and vegetables consumption for brain health.


DAIRY, BONE MINERAL DENSITY AND FRACTURES AND MENOPAUSE: Dairy consumption continues to be promoted as being ‘good for the bones’. However, there is very little scientific data to support this assumption. Yes, dairy is a source of calcium and vitamin D (when fortified), but that does not equate to benefits for bone health.
This study included participants from the The SWAN (Study of Women’s Health Across the Nation) cohort, composed of community based, multiethnic women across the menopause transition. The SWAN bone sub-study began baseline data collection in 1996, with 3,302 pre- or early peri-menopausal women aged between 42 and 53 years who had an intact uterus, at least one ovary, and no hormone usage in the last 3 months prior to screening from 5 clinical sites in the United States. After enrollment, women were followed annually for collection of information on demographic, clinical, and anthropometric data. 1955 participants were followed annually for 10 years, collecting data on bone mineral density and fractures. Menopausal status was based by annual questionnaire.
This study analyzed dietary data with a focus on dairy foods, which were divided into in four categories of total dairy foods of <0.5, 0.5 to <1.5, 1.5 to <2.5, and 2.5 servings/d or <1.5 and 1.5 servings/d. The results did not find any evidence of benefit for dairy intake on annualized rates of femoral neck and lumbar spine bone mineral density loss or risk of fractures. These findings are in line with 2 meta-analyses that also did not show a benefit for dairy consumption on hip fracture rates in men or women.
Get your calcium from whole plant foods and vitamin D from the sun (Vitamin D supplements are needed when sun exposure is not adequate)

If you have found this article useful, please follow my organisation ‘plant-based health professionals UK’ on Instagram @plantbasedhealthprofessionals and facebook. You can support our work by joining as a member or making a donation via the website
