Plant-based diets for the prevention and treatment of cardiovascular diseases
By Michael Metoudi, RD
What is cardiovascular disease?
Cardiovascular disease (CVD) defines a group of disorders affecting the heart and blood vessels. The most common type is coronary heart disease (CHD), characterised by the narrowing of blood vessels and reduced blood flow to the heart. If left untreated, it develops into other serious types of CVDs such as arrhythmias (irregular heartbeats), angina (chest pain), and eventually leading to myocardial infarction (heart attack) and heart failure. Other major types of CVDs include hypertension and cerebrovascular disease, such as stroke, both of which have significantly increased in the UK during the past two decades.
CVDs remain the commonest cause of illness and death worldwide. Alarmingly, the overall rates of heart disease have dramatically increased in younger people, suggesting that it is not just a disease confined to old age.
Risk factors for cardiovascular diseases
The main drivers of CVD are lifestyle-related and are mostly modifiable. These include:
1) Behaviour or lifestyle risks: such as poor dietary patterns, high in salt and low in whole plant foods; smoking; physical inactivity; and alcohol use.
2) Metabolic risks: such as high systolic blood pressure, obesity, high LDL-cholesterol and fasting blood glucose and diabetes.
3) Environmental risk: including air pollution.
Other emerging modifiable lifestyle factors include high stress levels, poor sleep and social isolation and loneliness. Genetics appear to be responsible for 40-60% of the risk for CVD. However, diet and lifestyle interventions can offset genetic risk for CVD by almost one half in susceptible individuals.
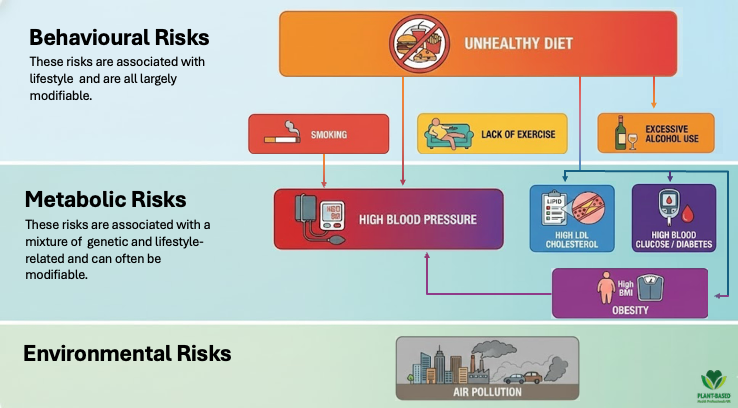
Cardiovascular disease risk factors
The evidence for whole-food plant-based diets in cardiovascular diseases
Prevention and Treatment
Poor diet quality represents the number one lifestyle risk factor for CVD, responsible for up to half of all cardiometabolic disease-related deaths.
Some of the strongest evidence supporting a whole food plant-based diet (WFPBD) for CVD relates to the prevention and treatment of CHD. Studies as far back as the 1950s have shown that predominantly and exclusively plant-based diets reduce CVD risk.
Two landmark cohort studies include the Framingham Heart study and the Seven Countries study, first linking diet quality (plant vs. animal fat) to CHD risk. Fast forward and we have over 75 years of data from meta-analyses of large prospective cohort studies consistently showing a reduced risk of CHD, overall CVD, their primary risk factors and CVD mortality in those following a plant-based diet. These studies include data from participants that follow vegetarian or vegan diets such as the EPIC-Oxford and Adventist Health studies showing just under 30% reduction for CHD.
For Intervention studies involving the primary prevention of CVD, the PREDIMED study showed that a Mediterranean diet pattern, supplemented with olive oil or nuts in those at high risk, reduced stroke and overall CVD events by at least one third. The more recent OMNIVEG study showed even greater benefits for heart disease risk factors for those following a vegan Mediterranean-style diet compared to the traditional Mediterranean diet.
When it comes to the treatment of established heart disease (secondary prevention), there are consistent and significant improvements in CVD risk factors including reduced blood lipids levels, blood pressure and markers of glycaemic control in people following a vegan or vegetarian diet.
The Lifestyle Heart Study, a randomised lifestyle intervention trial involved 48 patients with established CAD. This study showed that a predominantly WFPBD, low in fat, together with other lifestyle interventions (exercise, smoking cessation and stress management) resulted in 82% of patients showing regression of their arterial CHD in the intervention arm of the study, after 5 years of follow-up.
Importance of diet quality
Studies that consider diet quality, using the plant-based diet index, such as the Nurses’ Health Study and the Health Professionals Follow-up study, also find a similar risk reduction in CVD in those eating the highest portions of whole plant foods.
High adherence to a healthy plant-based diet is associated with a 14% reduction in CHD and a 10% reduction in overall CVD risk. Conversely, following an unhealthy plant-based diet, high in ultra-processed foods, refined grains, free sugars, unhealthy fats, and salt, can increase the risk of CVD and CVD Mortality.
When substituting animal foods for plant foods, such as nuts, legumes or whole grains, there is a significant reduction in CVD risk by as much as 30%. Fish consumption has also shown to reduce CVD risk up to 8%, but only in types with a high omega-3 fat content, suggesting this to be the primary cardioprotective factor. Adequate sources of omega-3 can be obtained in whole plant foods such as flaxseeds, chia seeds, walnuts, hemp hearts and soya.
Mechanisms that drive cardiovascular diseases
At the core (or heart!) of CVD is the development of atherosclerosis, the build up of plaque inside the arteries. These plaques are made up of predominantly fat, cholesterol, calcium and debris of cells from the immune system. Over time, these plaques harden, narrow the arteries, limit blood flow to the heart and organs and give rise to the collective symptoms of CVD. Plaque rupture leads to the formation of a blood clot, resulting in a myocardial infarction and/or stroke.
Atherosclerosis begins when specific lipoproteins, that transport lipids in the circulation (e.g cholesterol), become trapped beneath the endothelium that lines the blood vessels. Lipoproteins linked to this process include ApoB-containing lipoproteins, particularly LDL-cholesterol. Their retention within the arterial wall leads to an inflammatory reaction which drives the formation and growth of atherosclerotic plaques.
It is of great concern that the development of these plaques does not just occur later in life but appears to form even from early childhood.
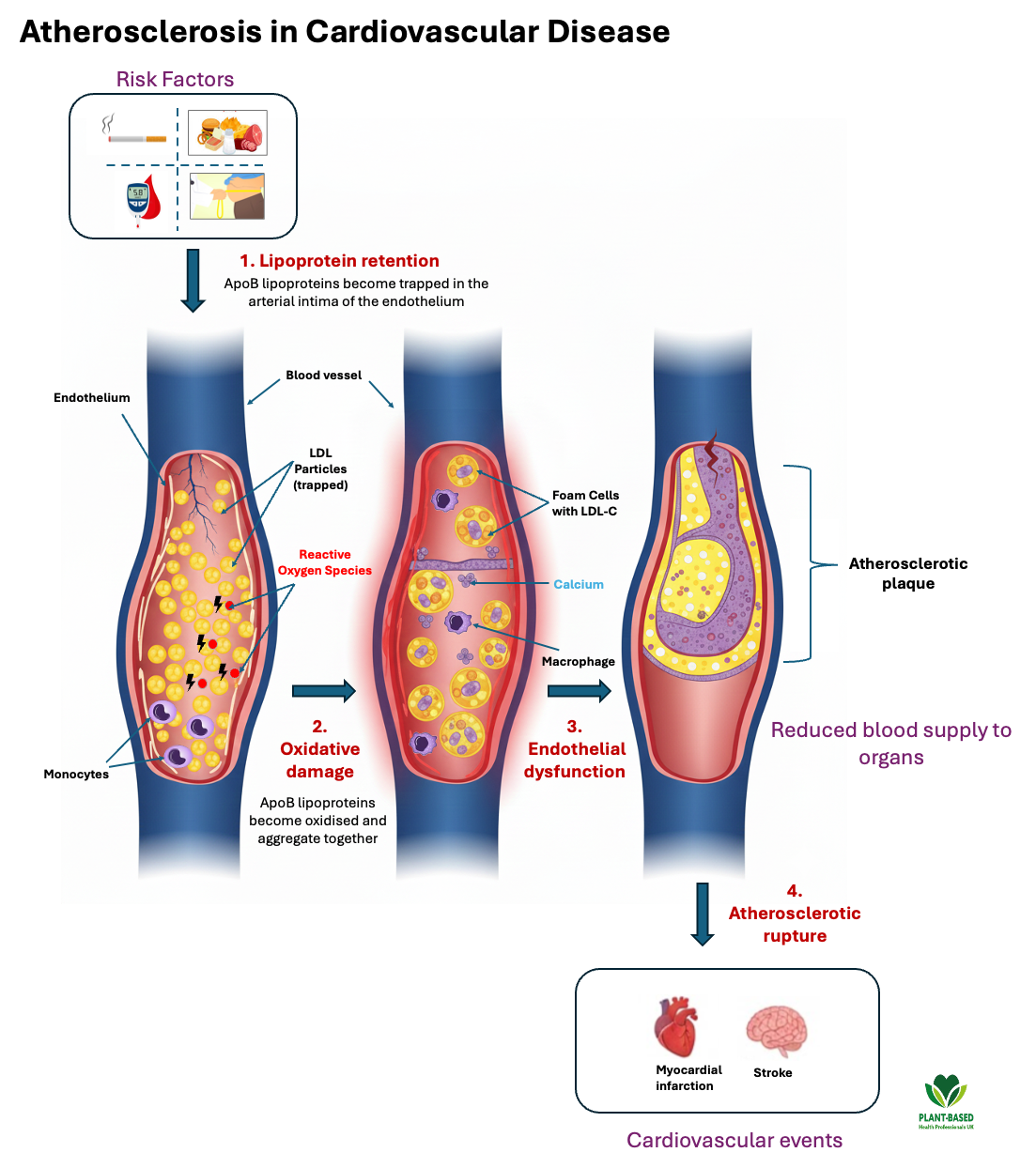
Atherosclerosis development in Cardiovascular Disease
How whole-food plant-based diets reduce cardiovascular diseases
Lowering blood pressure
High blood pressure, or hypertension, is the biggest risk factor for CVD. Several studies demonstrate the benefits of plant-predominant diets in reducing hypertension, with the DASH diet (Dietary Approaches to Stop Hypertension) most extensively studied. The core components of the DASH diet are fibre-rich plant foods and thus following a vegan or 100% plant-based diet has well-established benefits for lowering blood pressure. As the intake of animal-sourced foods are lowered and plant-based foods are increased, the greater the benefits for blood pressure lowering. Specific beneficial foods include whole grains foods, fruit and vegetables, and legumes.
WFPBDs are beneficial because of the abundance of dietary potassium, a mineral that is necessary for maintaining muscle function but also relaxing blood vessels, thereby reducing blood pressure. WFPBDs are naturally lower in salt, a major risk factor for hypertension. They are also higher in fibre, a nutrient consistently associated with blood-pressure lowering effects
Reducing blood and dietary lipids
Elevated blood lipids, especially LDL cholesterol, Lipoprotein (a)(LP(a)), a genetically-determined lipoprotein, and triglycerides are major risk factors for CVD. In general, the lower the levels of these lipids, the better for prevention and managing CVD. Saturated fat intake is the main determinant of LDL-cholesterol levels, with dietary cholesterol having a smaller, but still an important impact.
Vegetarians and vegans consistently have lower LDL-cholesterol levels than omnivores. There is a great deal of evidence based on the Portfolio diet, a combination of five plant-based food groups designed to lower cholesterol. These include plant sources of protein, nuts and seeds, sources of soluble fibre (oats, barley, psyllium), plant sterols and oils high in monounsaturated fats, such as extra virgin olive oil. (see our factsheet here). Despite Lp(a) being genetically determined, plant-based diets have also shown to reduce levels by as much as 16% in 4 weeks.
WFPBDs have a variable impact on blood triglycerides. However, fibre-rich plant foods have shown to significantly reduce levels, particularly nuts (rich in omega-3 fats) and whole grains. Minimising intake of free sugars and refined grains is also important.
Reducing inflammation and improving endothelial function
Plant-based diets lower the risk of CVD by reducing inflammation. Vegan and vegetarian diets as well as the Mediterranean diet were ranked highest for reducing C-reactive protein (hsCRP), a primary marker of inflammation that is linked to CVD by promoting atherosclerosis and endothelial dysfunction. Vegan and vegetarian diets appear to reduce other important circulating biomarkers of inflammation linked to CVD.
Whole plant foods have also directly been shown to improve endothelial function, especially through foods such as fruits, vegetables, soya, nuts and seeds, cocoa, and tea.
Blood glucose control and diabetes
Elevated blood glucose and type 2 diabetes almost doubles the risk of CVD, especially heart failure, heart attack and stroke. WFPBDs have shown to significantly reduce the risk of type 2 diabetes as well as having a role in the clinical treatment of type 2 diabetes. Emerging evidence also shows their role in the management of type 1 diabetes.
Modulating the microbiome
The gut microbiome is linked to a host of different diseases, with CVD being no exception. Specific species of gut bacteria appear to be responsible for an increased or decreased risk of CVD. Certain bacteria that metabolize compounds from carnitine, found in red meat and eggs produce trimethylamine (TMA), a molecule which gets converted to trimethylamine N-oxide (TMAO) within the liver. TMAO is linked to CVD risk. It can alter how cholesterol is metabolised by the body by disrupting reverse cholesterol transport and reducing its excretion, promoting lipid deposition, which accelerates atherosclerosis. Predominantly plant-based diets have shown to directly shift populations of gut bacteria from TMAO producers to beneficial bacteria that metabolise fibre and produce short chain fatty acids (SCFAs) that regulate blood pressure and reduce inflammation. Vegan diets in particular have gut microbiome signatures that are associated with improved cardiometabolic health.
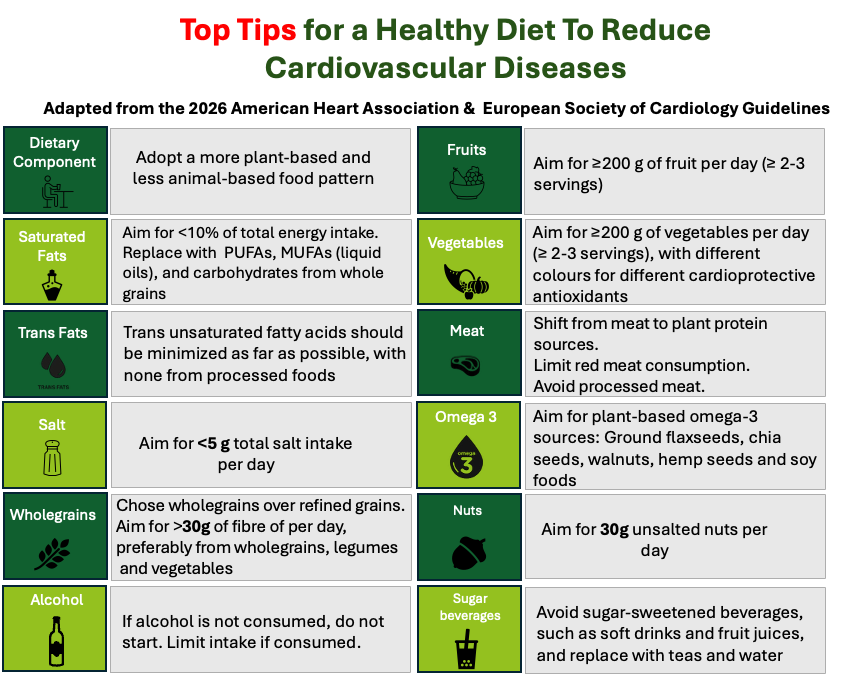
Consensus Guidelines for reducing Cardiovascular disease
Conclusion
There is an abundance of high quality evidence supporting a WFPBD for the prevention and treatment of CVDs. It addresses the root causes, whilst simultaneously providing the core nutrients that not only protect the heart and blood vessels, but do not contain the dietary components from animal foods that are directly linked to CVD risk, development and progression.
