A review of the week’s plant-based nutrition news 5th December 2021
This week I cover the 2021 Global Nutrition Report, the red meat trade and impact on health outcomes, effects of wine, chocolate and coffee consumption, plant-based diets and cardiovascular disease and nutrition education in medical schools.

GLOBAL NUTRITION REPORT 2021: This report makes for very sad reading. It clearly describes that globally we are way off course on dealing with the issues of malnutrition, which includes stunting, wasting and overweight/obesity. Worldwide, 149.2 million children under 5 years of age are stunted, 45.4 million are wasted and 38.9 million are overweight. Over 40% of all men and women (2.2 billion people) are now overweight or obese. Diet-related disease and mortality continues to rise with poor diets resulting in 1 in 4 deaths globally (26%). The proportion of premature deaths attributed to dietary risks is highest in Northern America and Europe (31% each), and lowest but also at notable levels in Africa (17%).
Diets remain insufficient in healthy plant foods, whilst being too high in meat, salt and sugar. Fruit and vegetable intake remains 50% below the recommended level of five servings per day that is considered healthy, and legume and nut intakes are each more than two thirds below the recommended two servings per day. In contrast, red and processed meat intake is on the rise and almost five times the maximum level of one serving per week, while the consumption of sugary drinks, which are not recommended in any amount, is going up as well.
The report finds that our food system continues to harm the planet creating more than a third (35%) of all greenhouse emissions and using substantial and rising amounts of environmental resources, with animal-sourced ‘foods’ responsible for the majority of greenhouse gas emissions and land use.
As a result, the cost to society of dealing with the consequences of our broken food system and unhealthy diets are astronomical and unsustainable. Therefore, we need urgent initiatives to transform food systems, increase the intake of health-promoting foods, and reduce animal-based ‘foods’, to ensure diets are healthy and sustainable for people and the planet. Of course, in high income countries, most of us don’t need to wait for these policy changes, we can immediately take action by changing our diet and focusing on plant-based foods.

NUTRITION EDUCATION FOR MEDICAL STUDENTS: One required urgent action as part of food system transformation is to incorporate more nutrition education into undergraduate healthcare and medical curricula. This has been recognised in the UK with the recently published nutrition curriculum and competencies for medical students. But how should the curriculum be implemented and which teaching methods are going to be effective at supporting clinicians incorporate nutrition counselling into their clinical practice?
I am proud to have supported our medical student member, Priya Patel, to publish her Masters project. This review is an update to the prior one published in 2017 that found a lack of adopted curricular standards for teaching clinical nutrition and that educators should consider including interprofessional education approaches, online learning, placing an emphasis on learners’ personal health behaviours, and standardised and real patient interactions.
Our review evaluated nutrition education interventions delivered to medical students and published between 2015 and 2020 in 15 papers. The analysis showed that most interventions were optional rather than compulsory for students and only four explicitly used interprofessional learning. There were however more novel methods used such as interactive cooking and some required students to teach their peers, school children or families about nutrition i.e. learning by teaching. However, content and evaluation of most interventions were heterogenous and there was difficulty identifying the impact of these interventions.
Overall, the study highlights the advantages of utilising interprofessional learning, focusing on student’s personal health behaviours and harnessing novel teaching methods such as hands-on cooking. It also highlights the need to use standardised, objective measures of outcomes and the need for a curricula-wide approach to integrating nutrition education.
At PBHP UK, Dr Hayley Tait, GP, chef and author is leading our latest project called ‘Cooking for the Climate’ and she is teaching hands on plant-based cooking to medical students at Exeter and Southampton University. We hope to be adding more medical schools to the programme very soon.

PLANT-BASED DIET AND CARDIOVASCULAR DISEASE (CVD): The most well established benefits of a plant-based diet are the impact on cardiovascular disease. Pretty useful given that CVD remains the top cause of mortality globally. We know that plant-based diets reduce the incidence of CVD risk factors including high blood pressure and cholesterol, overweight/obesity, type 2 diabetes and inflammation. It’s also useful to consider actual CVD outcomes such as incidence and mortality.
This paper brings together data from 13 cohort studies including 410,085 participants. These studies assessed the impact of a plant-based diet using the plant-based diet index and also included studies with vegetarian and vegan participants (78,672 in total).
The results showed that adherence to a healthy plant-based diet significantly reduced the risk of developing CVD (10.2% reduction) and dying from CVD (8.1%). In most studies vegetarians and vegans tend to be analysed together and there was a definite consistent reduction in CVD incidence, particularly seen in vegetarians, but impact on mortality was less obvious given the heterogeneity in diet quality. Unhealthy plant-based diets increased the risk of CVD.
The authors conclude ‘This study provides important evidence to suggest a possible protective role of plant-based dietary patterns against cardiovascular mortality and CVD among the general population’. Of note, a recent meta-analysis examining the effect of a vegetarian diet on CVD morality showed a 30% reduction in risk of death from ischaemic heart disease.
These facts alone provide sound evidence for promotion and implementation of a plant-based diet as the default diet for humans.

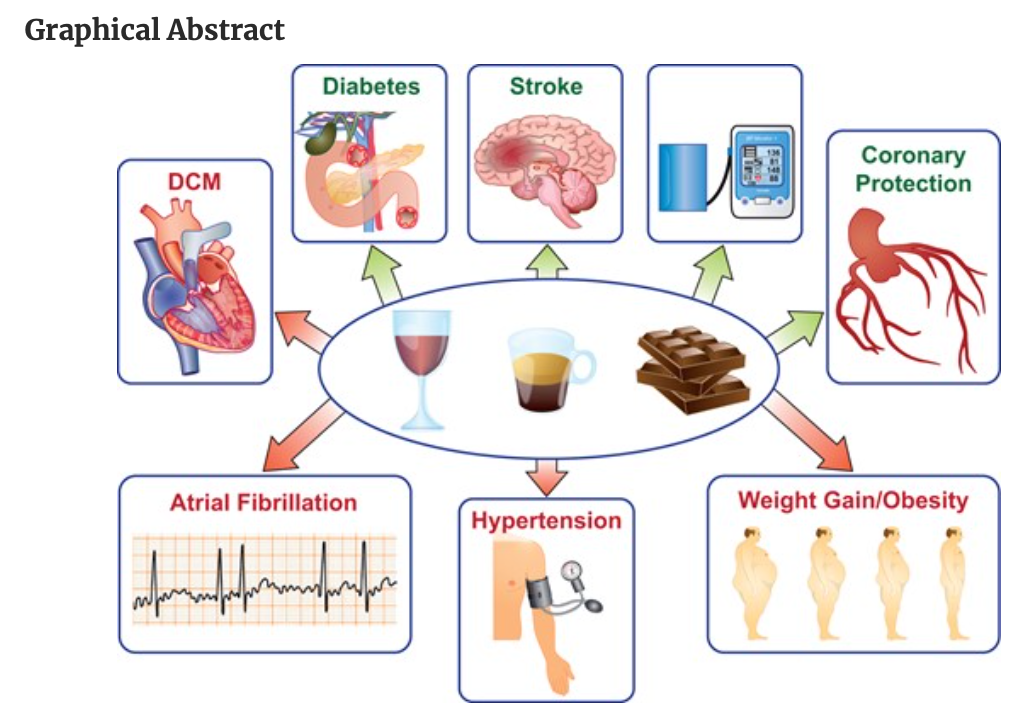
WINE, CHOCOLATE AND COFFEE: This is a nice, short, open access review of three dietary items often discussed amongst those on a plant-based diet. Food and drink can have varied effects in different scenarios and as always, the impact depends on the overall quality of the diet.
Overall, there is very little evidence for a benefit of wine consumption and concerns over adverse effects on brain health and cancer risk are greater. In contrast cacao beans have been associated with a number of benefits such as lower blood pressure, better endothelial health and positive effects on platelet function and insulin sensitivity. Of course, this relates to the consumption of dark chocolate (70% or more cacao) and not milk chocolate or varieties with more sugar than cacao. Overall, habitual coffee consumption, including decaffeinated versions, is associated with health benefits, protecting against cardiovascular disease, type 2 diabetes and chronic disease in general.
Chocolate and coffee are not necessary in the diet and these items may not suit everyone, but for those of us who do enjoy these, this is welcome news.

THE RED AND PROCESSED MEAT TRADE: If we are going to curb the continued rise in diet-related diseases, we need to address food production and trade first and foremost. This paper asked two questions:
(1) What is the impact of red and processed meat trade on diet-related non-communicable diseases (NCDs)?
(2) Which countries are particularly vulnerable to diet-related NCDs due to red and processed meat trade?
14 red meat and six processed meat items were selected and the authors investigated bilateral meat trade flows across 154 countries. The NCDs considered were ischaemic heart disease, colorectal cancer and type 2 diabetes.
The results showed that overall the global red and processed meat trade increased 148.4% when comparing the years 1993–1995 to 2016–2018. This increase in red and processed meat consumption with trade accounted for 10, 898 attributable deaths in 2016–2018, which was an increase of 74.6% when comparing deaths from 1993 to 1995. This was also associated with a significant increase in disability. A greater proportion of these deaths and disabilities were in developing countries compared to developed countries. Overall, 1.1–1.6% of all global deaths and disability are attributable to the red and processed meat trade.
The authors conclude ‘that global increases in red and processed meat trade contribute to the abrupt increase of diet-related NCDs, and the attributable burden of diet-related NCDs has large geographical variations among countries. To prevent unintended health consequences due to red and processed meat trade, future interventions need to urgently integrate health policies with agricultural and trade policies by cooperating between responsible exporting and importing countries’.
Health professionals need to play a major role in supporting patients and communities reduce and ultimately eliminate the consumption of red meat. Here is an article written by Dr Laura Freeman and myself for the BJGPlife magazine.
Please follow my organisation ‘plant-based health professionals UK’ on Instagram @plantbasedhealthprofessionals and facebook. You can support our work by joining as a member or making a donation via the website.
