A review of the week’s plant-based nutrition news 18th September 2022
A short review highlighting three new studies using the plant-based diet index to demonstrate the impact of a healthy plant-based diet.
THE PLANT-BASED DIET INDEX (PDI): I talk about this index a lot as it’s a useful way of understanding the impact of a healthy plant-based diet without the need to study large numbers of vegetarians and vegans. Created by researchers at Harvard University, the PDI can be used to score data from food frequency questionnaires and gives positive marks to all plant-based foods and negative marks to all animal-derived foods. The score has also been adapted to assess the impact of healthy versus unhealthy plant-based foods, with refined and processed plant foods also given negative marks. This creates a healthy plant-based diet index (hPDI) and an unhealthy plant-based diet index (uPDI).
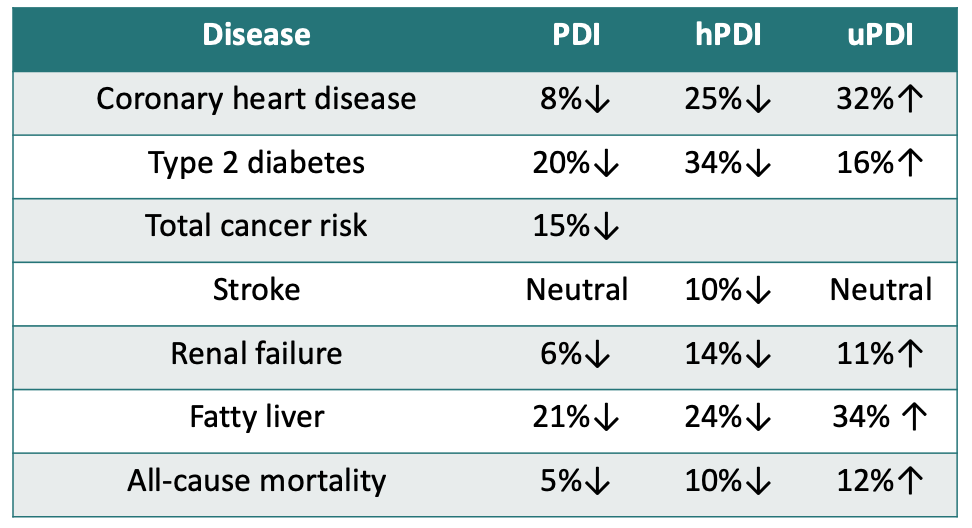
A number of studies have used this index and the data consistently shows that a healthy plant-based diet is associated with a significant reduction in the risk of a number of chronic conditions and also reduces the risk of premature death, whilst an unhealthy plant-based diet, high in refined grains and sugar, increases the risk. You can read more here. A summary of the data is shown below with references in the linked article.

PLANT-BASED DIET FOR ELDERS: There is often concern raised when older adults are following a plant-based diet. Caloric needs generally decrease with age but the requirements for some nutrients increase. For example, protein is less well absorbed and used less efficiently with ageing, regardless of diet pattern, and therefore there may be a higher protein requirement (1.0–1.2g/kg after age of 65 years). Older people synthesise vitamin D less efficiently from the sun and may spend less time outdoors and therefore are more likely to require supplements. Care should be taken to maintain calcium requirements and therefore it may be useful to incorporate fortified foods, such as plant-based milks and calcium-set tofu. Atrophic gastritis is common among people over the age of 50 years and can result in decreased absorption of vitamin B12 regardless of diet pattern, therefore B12 supplements are required as per any plant-based diet and some advocate for a higher dose with age. The sublingual route may also be preferable in order to bypass the stomach. Iron requirements in general decrease in post-menopausal women. The conversion rate of short chain omega-3 fatty acids to long chain decreases with age and it may be prudent to recommend higher intakes of ALA (at least 2.2 grams for females and 3.2 grams for males per day) and a micro-algae supplement. Overall, it is important to ensure that the foods being eaten are nutrient-dense, with a focus on a variety of healthy plant-based foods. There is also a natural loss of muscle mass (sarcopenia) with ageing and older people can be at risk of malnutrition. Overweight is an increasing issue and this can co-exist with low muscle mass.
Despite all these concerns, an increasing body of evidence supports plant-based diets for healthy ageing. Studies have shown that plant sources of protein are associated with a reduced risk of frailty compared to animal sources, with processed and unprocessed red meat in particular being associated with an increased risk of frailty.
This new study uses the PDI to assess the impact of a plant-based diet in community-dwelling older adults in Spain. Researchers analysed data from 1880 individuals with a median age of 68.7 years from the Spanish Seniors ENRICA-1 cohort. During the 3.3 years for follow-up, there were 136 cases of frailty. Those participants most adherent to a healthy plant-based diet had a 57% reduction in the risk of frailty compared to those who were least adherent. Participants consuming the most unhealthy plant foods as per the uPDI had a 289% increased risk of frailty.
Regarding individual foods, vegetables, vegetables oils and fish/seafood were associated with a lower risk of frailty. Of note however, data on how much of each food participants were consuming has not been provided, therefore it is not clear whether some foods, such as beans, were actually being consumed at high levels.
There are several reasons why a diet high in healthy plant-based foods would be associated with a lower risk of frailty. This type of diet pattern is rich in fibre, antioxidants and anti-inflammatory compounds. It supports better gut health and reduces the risk of other chronic condition. More data on 100% plant-based diets for elders would be beneficial.

PLANT-BASED DIETS FOR SOUTH ASIANS: South Asians are more likely than other ethnic groups to consume a vegetarian diet, yet people from the South Asian subcontinent have a greatly increased risk of cardiometabolic conditions compared to Whites and on average develop conditions such as type 2 diabetes and cardiovascular disease 10 years earlier. Thus, understanding the impact of diet on the risk of chronic conditions is vitally important given that it is a significant modifiable risk factor.
This study analysed data from 891 participants of South Asian ancestry in the Mediators of Atherosclerosis in South Asians Living in America (MASALA) study. Overall, the results showed that adherence to a healthy plant-based diet, as defined by the hPDI, was associated with significantly better cardiometabolic health, including lower fasting glucose levels, improved insulin sensitivity, lower LDL-cholesterol levels, lower body weight, less visceral fat, lower levels of inflammation (high sensitivity CRP — although this lost significance after adjustment for BMI) and higher levels of adiponectin (a fat-derived hormone that protects against diabetes and atherosclerosis). Of note. For each 5-unit higher hPDI score, there was an 18% lower risk of type 2 diabetes. The opposite was true for an unhealthy plant-based diet, which in general was associated with worse cardiometabolic health.
This is an important dietary study for people of South Asian descent, as there are limited options available for prevention of cardiometabolic diseases that do not involve pharmaceuticals. The authors conclude ‘while consuming an overall plant-based diet was associated with lower cardiometabolic risks, the risks were much lower for those consuming a healthy plant–based diet. Future intervention and policy efforts to lower cardiometabolic risks in this high-risk population should focus on promoting a healthy plant–based diet, since it is associated with better health outcomes and is also environmentally sustainable’.

PLANT-BASED DIETS AND OBESITY: We have known for many years that people eating a meat-free diet tend to have a lower body weight, with vegans having the lowest BMI of all diet patterns. This is one of the major advantages of a plant-based diet as foods consumed tend to be low in calorie density yet nutrient-rich. You can read my article on plant-based diets and body weight here.
It is good to see this study, which brings together data from 9 prospective cohort studies that have used the PDI to assess the impact of plant-based diets on weight management. All studies were conducted in Western populations except for one study in South Korea
The results confirm that adherence to a plant-based diet is associated with lower body weight, with a greater impact when a healthy plant-based diet is followed. However, the uPDI showed that a diet composed of unhealthy plant foods had no advantage for body weight.
The authors conclude ‘A healthful plant-based diet provides a framework that can be used to create individualised diets that are socio-culturally appropriate, acceptable, and sustainable for lifelong health that reside within planetary health boundaries’.
Please follow my organisation ‘plant-based health professionals UK’ on Instagram @plantbasedhealthprofessionals and facebook. You can support our work by joining as a member or making a donation via the website.
