A review of the week’s plant-based nutrition news 28th June 2020
More nutrition controversy this week with a proposal to remove guidance on limiting saturated fat in the diet.

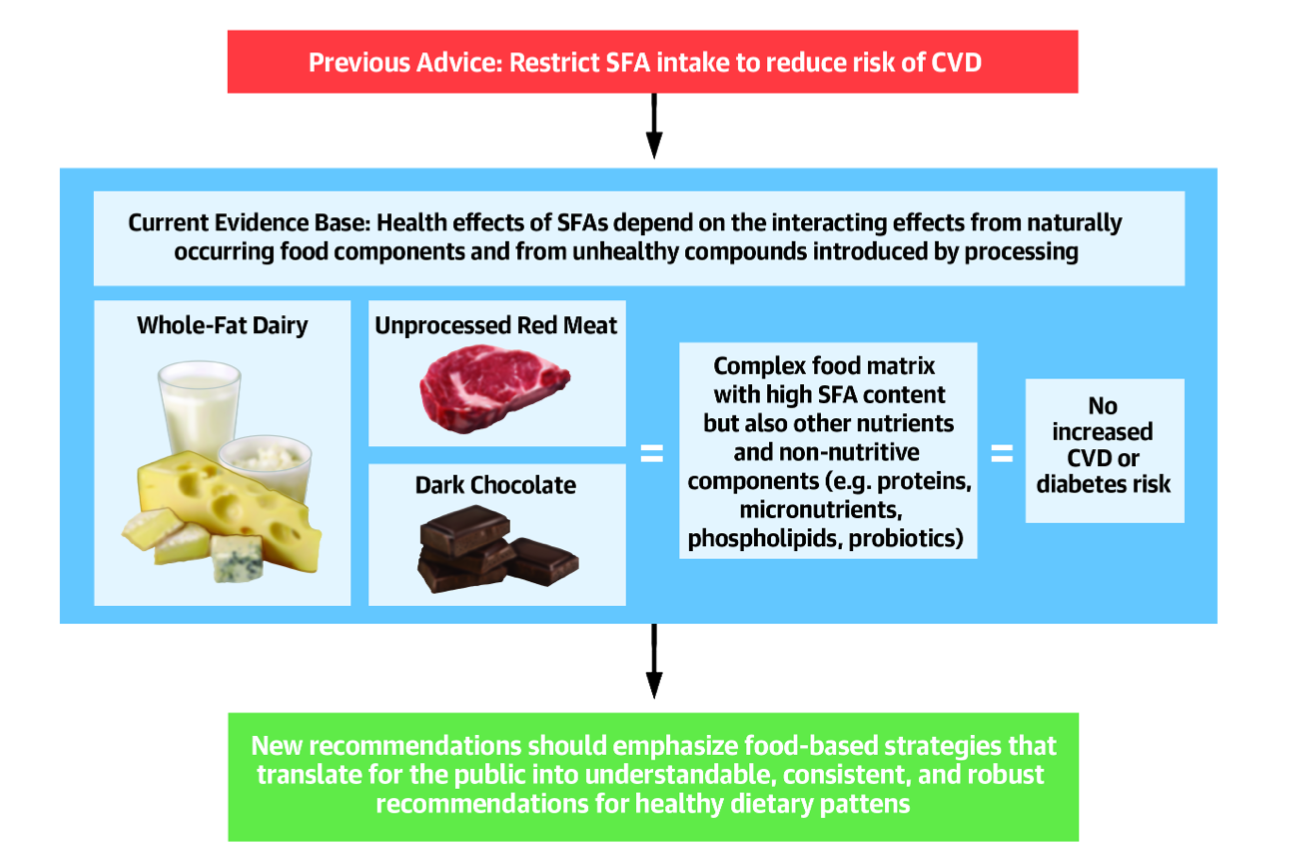
I AM IN UTTER SHOCK AND DISBELIEF — WHY ? A pre proof article has been published by no other than the American College of Cardiology making recommendations to abandon guidelines on limiting saturated fatty acid (SFA) intake and to encourage the consumption of whole-fat dairy, unprocessed meat (including red meat), eggs and dark chocolate. This is published by the same organisation that recommends a plant-based or Mediterranean diet for the primary prevention of cardiovascular disease (CVD). There much be something ‘vishy’ about this new paper! Here are a few things to consider.
1) 8 of 11 authors are either funded by the dairy or meat industries or receive money through the promotion of low carb/high fat diets. The umbrella organisation, the nutrition coalition, supporting these proposals consists of a group of low carbohydrate advocates. Now of course you could criticise me for being a vegan advocate and henced also presenting a biased view point. However, I do not directly receive a salary from any vegan or plant-based organisation. If I stopped my work in the plant-based movement today, I would not suffer any financial consequence and would only free up a lot of time! I work for the NHS and for Winchester University. That is it. I also do not tell my patients to go vegan. I tell them a healthy diet is one centred predominantly around whole plant foods.
2) There is no new science, just reinterpretation of existing data. The paper once again states that most recent meta-analyses of randomized trials and observational studies found no beneficial effects of reducing SFA intake on CVD and total mortality. This is true, but these meta-analyses have a number of flaws. They don’t consider what is replacing saturated fat in the diet i.e. refined sugars/grains are just as bad for health, and they do not consider large enough changes in SFA intake. Small changes in SFA consumption only lead to small, often non-significant effects on health.
This is the alternative argument. A Cochrane review, with no ties to Industry, published that cutting down on saturated fat consumption over a 2 year period led to a 21% reduction in the risk of CVD (including heart disease and strokes). Although there was no impact on the risk of dying, to reduce CVD risk by 21% is not to be ignored. Impact on mortality is always difficult to show due to better and more sophisticated medical therapies that have improved survival from CVD . The review showed that the greater the reduction in SFA intake the greater the effect on blood cholesterol and the greater the benefit for CV health.
The diet pattern with the lowest intake of SFA is a 100% plant-based diet or a healthy vegan diet. A healthy plant based diet has been shown to reduce the risk of coronary heart disease by 25%. The most recent meta-analysis of vegetarian and vegan diets has shown a 25% reduced risk of ischaemic heart disease in vegetaraians. These facts were not mentioned in the review paper.
3) The results of the PURE (prospective urban rural epidemiological) study are given considerable weight. But this study merely highlighted the impact of socioeconomic disadvantage on health outcomes. People in low income countries are more likely to have poor nutrition, eat more refined grains, have less access to healthcare and hence worse health outcomes. To suggest that better health outcomes in high incomes countries relates to higher SFA intake seems an overstretch. Many have written about the flaws of this study, including myself.
4) The results of ‘low fat’ interventions such as the Women’s Health Initiative (WHI) and the PREDIMED study are cited as evidence of failure of low fat interventions. But in neither of these studies was a low fat diet achieved. The aim of the WHI study was to reduce fat intake to <20% of calories but the median fat intake in interventation group remained between 20–30% of calories with only an 8% reduction in total fat and a 3% reduction in saturated fat compared with the control group. In the PREDIMED study the control arm had a total fat intake of over 30% of calories and the saturated fat intake did not differ between the control and the intervention arms.
A truly low fat intervention is one that aims to lower total fat intake to 10–15% of total calories and saturated fat intake to <7% of calories. Such studies involve eating a predominantly or entirely plant-based diet. Both Dr Dean Ornish and Dr Caldwell Esselstyn have shown such a diet to have the potential to arrest and reverse ischaemic heart disease.
5) The real life North Karelia project in Finland was a community intervention to reduce the alarmingly high death rate from heart disease in the region. Started in 1972, the aim was to improve cardiovascular risk factors such as blood cholesterol, blood pressure and stop tobacco smoking through a diet and lifestyle intervention and medications when needed. The diet changes involved drastically cutting the SFA intake of the population and increasing the consumption of whole plant foods. The intervention was a remarkable achievement and led to a >80% reduced risk of dying from heart disease in men over a 30 year period.

6) The scientific advisory committee on nutrition in the UK has reviewed the evidence on SFA consumption and its advice from August 2019 confirms that limiting saturated fat intake has benefits for health.
7) This is the best line in the whole review ‘The ability of adult humans to digest the sugar unique to milk, lactose, evolved separately numerous times, demonstrating unequivocally that the ancestors of many modern humans required continuous dairy consumption for survival to reproductive age’.
So what about the 70% of the worlds population that does not have lactase persistence and are therefore intolerant of lactose beyond weaning? Is this not a rather racist statement given lactose tolerance and adaptation is mainly a white, European phenomenon? A recent ‘state of the art’ review on Milk and Health summarises the entirety of the data on the subject and it is clear that dairy consumption is not essential to health, does not provide protection from osteoporosis, overweight or cardiovascular disease and may even cause harm.
8) I do agree that we should be advising based on foods not nutrients. But the food and diet patterns associated with the longest healthiest lives are centred around fruits, vegetables, whole grains, legumes nuts and seeds i.e. Mediterranean, DASH, vegetarian and vegan diets. They minimise red meat and processed foods. To suggest otherwise is mis-representing the data.
9) To encourage foods such as unprocessed red meat, eggs and dairy that are unsustainable for planetary health is totally irresponsible. The only way we are going to survive on planet earth as a global community of almost 8 billion people is if we shift to a plant predominant way of eating. This will be win win for our health, the planet and the animals.

BENEFITS OF A VEGETARIAN DIET PATTERN: In complete contrast to the first article, this editorial, accompanies a series of papers on vegetarian diets and health in the journal Frontiers in Nutrition. It summarises the main themes of the series and our current knowledge on plant-based diets — both vegetarian and vegan. The points made include the following; High quality vegetarian diets — that is one centred around whole plant foods and minimises processed foods — are associated with significant reductions in cardiovascular disease, without the side effects of medication; This may then also help reduce society’s health care costs; Fruit consumption is associated with better weight management and plant-based diets in general are associated with a more healthy BMI, which helps to reduce the risk of type 2 diabetes; Plant-based diets for rheumatoid arthritis are reviewed with evidence suggesting the potential for benefit due to its anti-inflammatory properties and its benefits to gut health; Vegetarian and vegan diets have a number of benefits for gut microbiome by creating a more diverse and stable gut ecosystem and increasing the short-chain fatty acid (SCFA) producing bacteria; The SCFAs improve immune function, blood-brain barrier integrity, increase insulin sensitivity and have cardio-protective effects; We are reminded that vegetarian diets reduce our exposure to pesticides and herbicides as they are lipophilic and therefore accumulate in fat of food animals. The bioaccumulation of pesticides can have harmful effects on animals, as well as people who consume meat and dairy.
The editorial concludes ‘Arguments for diverse health benefits of high-quality vegetarian diets are thus varied and robust. They are, as well, timely – as meat consumption is a major consideration in an array of threats to planetary health’. We must remember that the environmental and climate effects of food at scale are relevant to health outcomes in humans and without a healthy planet there will be no healthy people.
VEGETARIAN DIETS IN ADOLESCENTS: This paper forms part of the special series of article in the Frontiers of Nutrition Journal and provides data on diet quality in vegetarian adolescents. The study used data from the cross-sectional Teen Food and Development Study conducted among adolescents to examine associations between dietary intake and health outcomes. It included 601 participants (262 males and 339 females) aged 12–18 years old in a predominantly Adventist population in the US. The Adventists are a group known to follow a healthy lifestyle that many also include a plant-based diet. This study described and compared the dietary intake of vegetarian and non-vegetarian adolescents and also compared dietary intake with the general US adolescent population.Vegetarians were defined as the combined intake of meat, meat derivatives, poultry, and fish of <1 serving per week.
As expected, vegetarians consumed significantly more plant-based foods, meat alternatives, and dairy substitutes compared to non-vegetarians. Vegetarians also consumed higher amounts of most nutrients except those that are associated with animal foods (total fat, SFA, animal proteins, and zinc). In comparison to the general US adolescent population, both groups had a better diet quality. About half of vegetarians but just 25% of non-vegetarians met the recommendation for saturated fat intake of <10% of total energy intake, while over half of vegetarians and about one-third of non-vegetarians met the dietary fibre recommendation. Overall, vegetarians had greater intakes of foods considered to be beneficial to health and had better nutrient intake profile, including lower intakes of energy and SFA, a more favorable omega-6 to omega-3 ratio, and higher intakes of dietary fibre and most nutrients of concern — folate, iron, and the bone minerals calcium, potassium, and magnesium. A finding of concern was that the majority of both diet groups (82% of non-vegetarians and 84% of vegetarians) exceeded the recommended upper limit (2,200 mg for ages 9–13 and 2,300 mg for ages 14–18) of sodium. Most of this variation in salt intake was found to be due to consumption of bread/pasta/grains.
The study demonstrated that vegetarian adolescents had a more favourable dietary pattern than non-vegetarians and it is thought that this could translate into better health in adulthood, but further studies are required to confirm this. The high salt intake is a concern and should be addressed. This study adds to the slowly increasing knowledge we have on the adequacy of plant-based diets to meet the nutritional needs of children with no detriment to health.

TYPE 2 DIABETES (T2D) REMISSION: This is a much needed document from the American College of Lifestyle Medicine. The position paper clarifies that we now have enough data to recommend that remission with the use of intenstive lifestyle interventations should be the clinical goal in T2D treatment. The optimal treatment to bring about remission includes a whole food, plant-based (WFPB) dietary pattern coupled with moderate exercise. Remission is defined as achieving glycaemia below the diabetic range in the absence of active pharmacologic or surgical therapy for at least 1 year. Based on the studies reviewed, physical activity has less of an impact on remission induction when compared to diets. Studies show that remission is possible in the majority of people if T2D has been present for less than 8 years and if the lifestyle intervention is intensive enough.
There are a number of ways to acheive remssion. The most established is weight loss using a low calorie meal plan or low calorie meal-replacements but this needs to be followed by a careful reintroduction of a sustainable and healthy diet. A low-carb diet has also been shown to induce remission but there are concerns over the long term adverse effects of this approach, especially if carbohydrates are being replaced by animal sources of fat and protein. A whole food plant-based diets appears to be a more sustainable and practical approach with potential for longer term benefits for cardiovascular health and cancer prevention.

DIET, INFLAMMATION AND CANCER: At the core of all chronic diseases is the underlying mechanism of inflammation. Cancer is no different. Diet and lifestyle behaviours can promote or prevent inflammation. There are different ways of analysing diet patterns and scores are given to different foods and nutrients. A recently developed scoring system to summarize the inflammatory potential of multiple dietary components is the Dietary Inflammatory Index (DII), which assigns inflammatory weights to different foods components according to their proinflammatory or anti-inflammatory properties. Higher/more positive DII scores reflect more proinflammatory diets and lower/ more negative scores reflect more anti-inflammatory diets. No surprise that red and processed meat score positive marks and fruits and vegetables negative marks. Higher DII scores have been associated with higher levels of inflammatory biomarkers and an increased risk of several chronic diseases, including certain cancers. The actual scoring is pretty complex shown in the table below from the original article that developed the score.
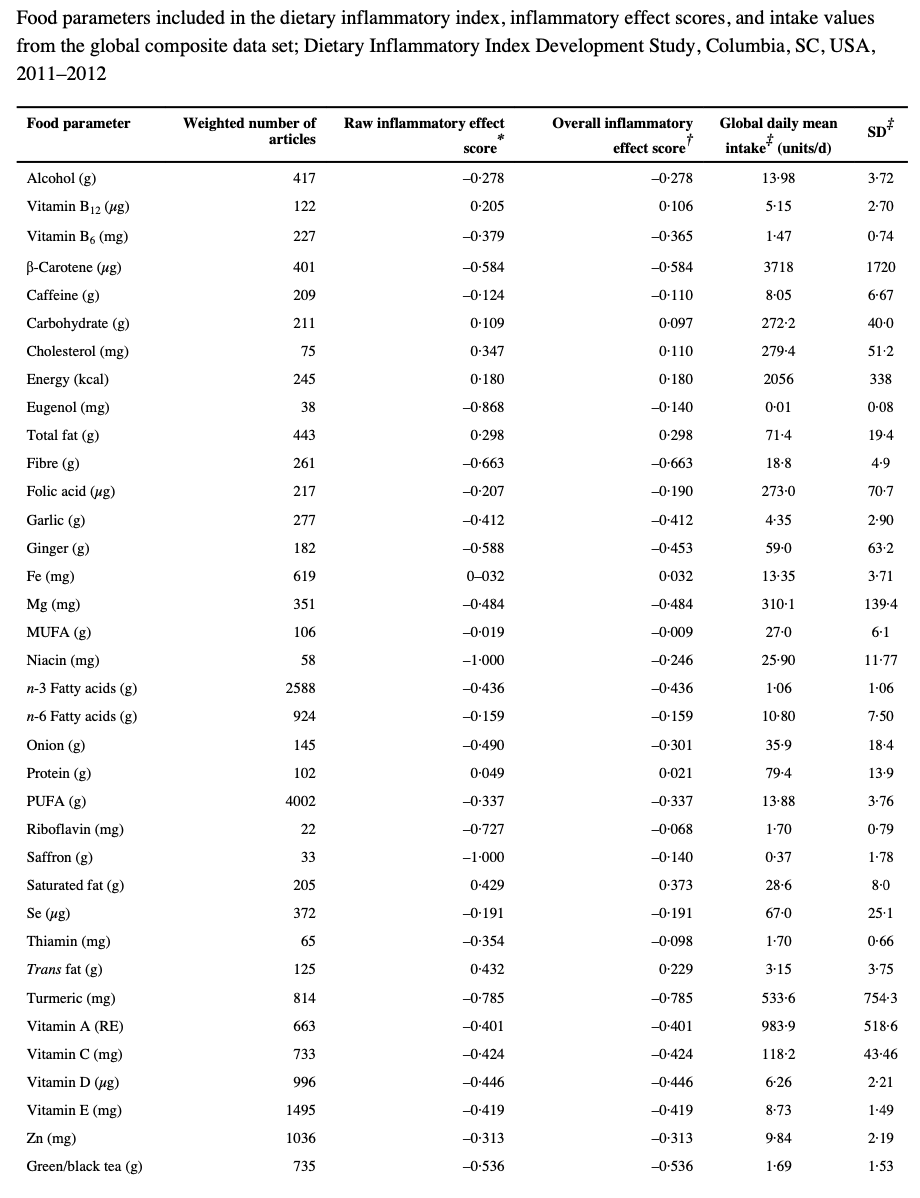

The paper highlighted reports data from the EPIC study. This is one of the largest prospective cohort studies ever to study the impact of diet on cancer. It finds that a higher DII is associated with a significant increase in colorectal cancer, particularly in men. In addition, the risk was further increased by combining obesity and lack of physical activity, both risk factors associated with inflammation.
We know from several prior studies that a plant-based diet effectively minimises the dietary impact of inflammation. The array of phytonutrients all act to keep inflammation in check. A vegan diet has been shown to significantly reduce markers of inflammation in the blood.

If you have found this article useful, please follow my organisation ‘plant-based health professionals UK’ on Instagram @plantbasedhealthprofessionals and facebook. You can support our work by joining as a member or making a donation via the website.
