Review of the plant-based nutrition news August 2023; a focus on cancer.
This month I focus on diet and cancer, ahead of my talk at the VegMed conference in September and to mark the launch of our new short course on cancer at University of Winchester.
Many people still believe that cancer is genetic and that it’s an inevitable part of life. This is only true for a minority of cancers. Less than 10% of cases are caused by the genes we inherit from our parents. Cancer cells do display abnormalities in their genes and chromosomes, which gives them the characteristics we associate with cancer, but these genetic defects are usually acquired during life for a variety of reasons. Many of these reasons relate to our diet, lifestyle and environmental exposures.
In 1981, Sir Richard Doll and his colleague Richard Peto at Oxford University submitted a landmark report commissioned by the US congress. The aim of the research report was to determine the percentage of cancers caused by avoidable risk factors. The article became a reference standard for estimates of the relative roles of lifestyle versus environmental versus host factors as causes of cancer in the US population. The report identified that up to 90% of cancer could be prevented by addressing lifestyle and environmental factors. The strongest and most certain cancer risk factor at the time was tobacco, accounting for 30% of cancer deaths. Other important risk factors identified by Doll and Peto were diet, estimated to be contributing to 35% of cancer deaths, alcohol, sexual behaviours, infections, occupational and industrial exposures, pollution and medicine and medical procedures.
A review of the original report published in 2015 found that Doll and Peto’s estimates of cancer risk have held true over the intervening 35 years and that the vast majority of cancers could be prevented by addressing lifestyle and environmental factors.
The latest estimate from the Global Burden of Disease Study Group finds that globally 40–50% of all cancers could be prevented by addressing modifiable risk factors. The leading risk factors are tobacco smoking, alcohol consumption, excess body weight, unsafe sex, dietary risk factors and high fasting plasma glucose.
The World Cancer Research Fund and American Cancer Society guidelines on cancer prevention provide 9 recommendations that together have the ability to reduce the risk of cancer by 40%. Five of the recommendations are dietary. Adherence to these guidelines, when analysing data from prospective cohort studies, does result in a significant reduction in cancer risk, even if followed imperfectly. Each additional risk factor which is addressed has an additive effect on cancer risk. Making the necessary lifestyle changes such as reducing body weight when required, stopping smoking and drinking alcohol and adopting regular physical activity will also overtime result in a reduced cancer risk. So it is never too late to make these changes. There is also good evidence that these recommendations should be followed by people living with cancer and that this can improve cancer outcomes, such as remission duration and survival.

In the UK, one in 2 people will develop cancer in their lifetime. In the UK and US it is estimated that around 1 in 20 (5%) of cancers are caused by an unhealthy diet, but these estimates do not fully take into account the role of dietary risk factors in causing overweight and obesity, type 2 diabetes and other chronic conditions that elevate the risk of cancer.

EARLY-ONSET CANCER IS RISING: Worryingly, cancer in people under the age of 50 years is rising. This is especially true for cancer of the gastrointestinal tract. The reasons for the rise in risk of early-onset cancer are not yet fully understood, but changing exposure to risk factors is considered a major contributor. Since the mid-20th century, there have been substantial changes in diet, lifestyle, environmental exposures, rates of obesity and changes to the health of the microbiome. All of these risk factors may interact with genetic susceptibilities, leading to an earlier onset of certain cancers. Considering the long latency periods of cancer development, risk factor exposure in early life (from conception to adolescence) and during young adulthood are considered to play a key role in the development of early-onset cancer.

FOOD DESSERTS, OBESITY AND CANCER: Data on cancer deaths highlights the impact that unhealthy food environments have on health outcomes and the contribution to health inequity. In this study from the US, researchers assessed the association between so called ‘food deserts’ (geographic areas where residents have few to no convenient options for securing affordable and healthy foods — especially fresh fruits and vegetables) and food swamps (ratio of fast-food and convenience stores to grocery stores and farmers markets) with obesity-related cancer deaths.
The results showed that there was a 77% increased risk of obesity-related cancer death in areas deemed to be food deserts or swamps, with a clear dose effect. Obesity-related cancer deaths occurred more frequently in people of Black ethnicity, those living in greater poverty and people with type 2 diabetes.
We are not doing much better in the UK in terms of access to healthy food and rates of obesity. The 2023 Broken Plate report from the Food Foundation makes for stark reading. People of lower economic means are unable to access healthy, nutritious food and are much more likely to be overweight or obese, an issue that is increasingly prevalent in our children. After smoking, obesity is the second most common preventable risk factor for developing cancer.

ULTRA-PROCESSED FOOD AND CANCER: This is still an emerging story, but the precautionary principle should apply. In the UK and US, more than 50% of food consumed by adults and children is classified as being ultra-processed. We know that these foods contribute to overweight and obesity and increase the risk of cardiovascular disease and type 2 diabetes.
In the last few years, data have been emerging that the consumption of ultra-processed foods (UPF) may also increase the risk of developing cancer. The first prospective study to show this came from France and the NutriNet-Santé cohort. The data showed that for every 10% increase in consumption of UPFs there was an associated 10% of more increased risk of developing any cancer and also breast cancer specifically. This current systematic review and meta-analysis brings together the available data from 11 studies, including eight retrospective case-control studies and three prospective cohorts. The results showed a consistent, dose-dependent increase in risk of cancer. For every 10% increase in UPF consumption there was a 13% increase risk of all cancers. There were specific associations with breast cancer (11% increase), colorectal cancer (30% increase) and pancreatic cancer (49% increase).
There are numerous reasons why UPFs could be contributing to cancer risk. The additive and preservatives themselves, exposure to toxins within the food packaging, the lack of healthful, cancer preventing nutrients such as fibre, anti-oxidant and anti-inflammatory compounds, exposure to processed meat (a known group 1 carcinogen) and of course adverse changes to the gut microbiome.

PLANT-BASED DIETS REDUCE RISK OF CANCER: We have known for over a century that a meat-heavy diet increases the risk of cancer. It is interesting to note that when cancer risk was accessed across 191 mammalian species by analysing post-mortem records for 110,148 animals that died in zoos, it was found that the ‘distribution of cancer mortality is associated with diet, with carnivorous mammals (especially mammal-consuming ones) facing the highest cancer-related mortality’. These findings were independent of body mass and life expectancy. The authors suggest that this may be due exposure to viruses and pollutants, low fibre and high fat consumption and negative impacts on the gut microbiome of high meat diets.
In contrast, there is now an abundance of data supporting plant-based dietary patterns, including vegetarian and vegan, for reducing the risk of cancer. Data from the EPIC-Oxford study showed that vegetarians and vegans had a 11% and 19% reduction in overall cancer risk respectively. In the Adventist Health Study-2, vegetarians and vegans had a 8% and 16% reduction in risk, respectively. Data are mixed when it comes to specific cancer subtypes. More recently, data from the UK biobank shows that people on a meat-free diet had a 14% reduction in all cancers, with greater reductions for breast and prostate cancer.
Plant-based diets are particularly beneficial for reducing the risk of cancers of the gastrointestinal tract. In a meta-analysis of studies, including more than 3 million participants, a variety of plant-based dietary patterns, including vegetarian and vegan, showed a significant reduction in a number of digestive cancers, including colo-rectal (24% reduction), pancreatic (29% reduction), gastric (19% reduction) and liver (49% reduction).
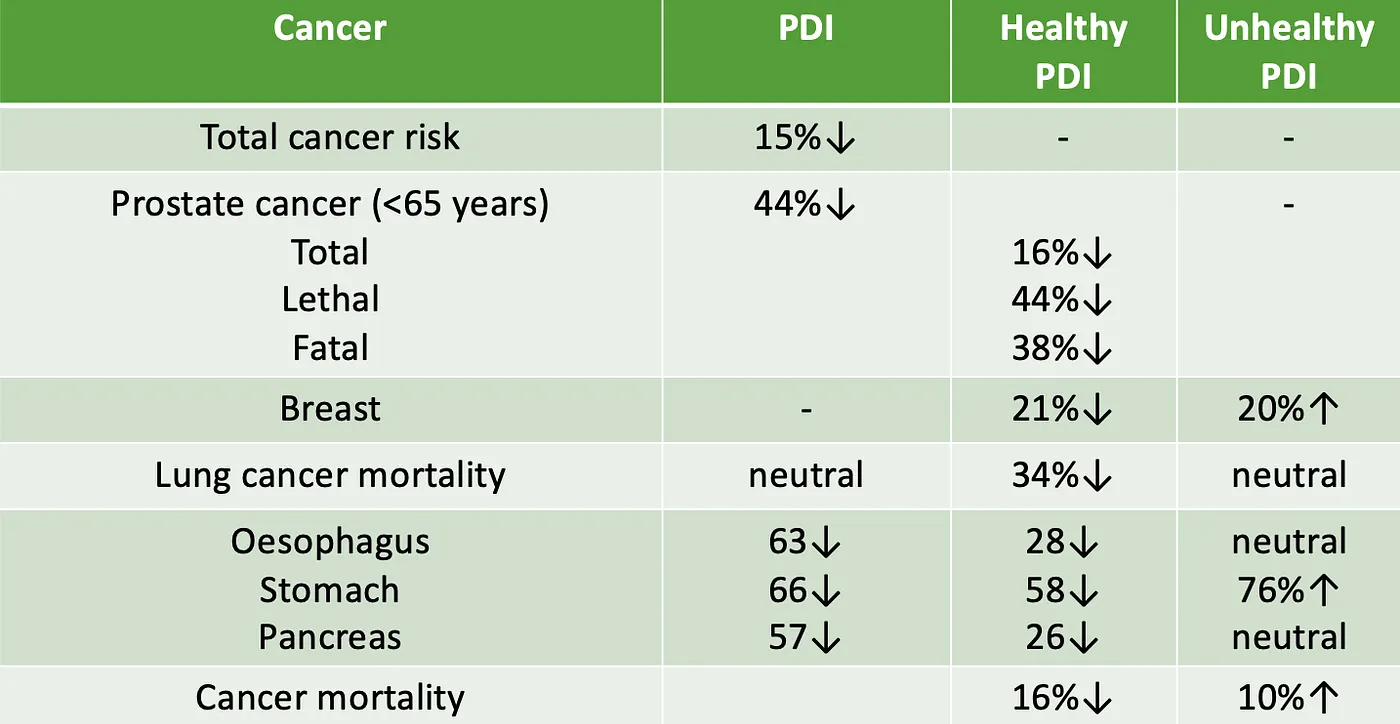
My favourite plant-based dietary index has been used to assess the impact of healthy plant-based diets on cancer risk using population data. When first used to analysis data from the NutriNet-Santé cohort, a healthy plant-based diet reduced the overall risk of cancer by 15%. Since then numerous studies have been published to show the widespread benefit of a healthy plant-based diet on site-specific and overall cancer risk. I have summarised recent data in the image above.

PLANT-BASED DIETS AND DIGESTIVE CANCER: A new analysis from the Nurses’ Health Study and the Health Professionals Follow-up study, with more than 200,000 participants followed for over 30 years, once again demonstrates the benefits of a healthy plant-based diet for preventing cancers of the gastrointestinal tract. There was a dose-dependent relationship, with the more healthy plant foods consumed the lower the risk. In contrast, an unhealthy plant-based diet, high in processed foods, sugar and refined grains increased the risk of gastrointestinal cancers with a dose effect.

CANCER AND THE GUT MICROBIOME: The most exciting field of nutritional research at the moment, is using dietary modification to improve the health of the gut microbiome. This is because the health of the gut microbiome has been shown to be a predictor of response to and survival after a number of cancer treatment, especially those treatments that harness the power of the persons own immune system i.e. immunotherapy.
For example, a study of 52 people with cancer receiving immunotherapy demonstrated that the higher the concentration of SCFA’s in the faeces, a marker of gut microbial health, the longer the remission after treatment. In this study, higher intakes of fibre-rich foods such as green vegetables, cabbage, and mushrooms, were associated with higher concentrations of faecal SCFAs. In people with melanoma receiving immunotherapy, dietary fibre intake was predictive of response to immunotherapy, with every 5-g increase in daily dietary fibre intake corresponding to a 30% lower risk of progression or death. Of note, in this same study, use of probiotic supplements was of not benefit and seemed to counteract the beneficial impact of the higher fibre intakes. In a study assessing dietary patterns and response to immunotherapy in people with melanoma, those most adherent to a Mediterranean-style diet, rich in fruit, vegetables, whole grains, beans, nuts and fish, had a better response to treatment and longer remission. Taken together, these studies show that a healthy diet pattern, centred around fibre-rich foods support a healthier gut microbiome which may have a positive impact on responses to anti-cancer treatments. To take this one step further, a first in man study of faecal microbial transplant showed that the transfer of faeces from a person whose cancer had responded to immunotherapy into a person who had previously not responded, helped promote a better response in that individual.
The gut microbiome has also been shown to be important in haematological cancers. This was first reported in the setting of stem cell transplantation, whereby a healthier gut microbiome was predictive of a lower risk of death from the procedure and subsequent studies suggest the health of the gut microbiome may impact rates of graft versus host disease — the rejection reaction that occurs after stem cell transplantation. Similarly, adverse changes in the gut microbiome may influence response and complications from treatment for diffuse large B-cell lymphoma, the commonest type of lymphoma.
Dietary modification seems to be a sensible first step in promoting a healthier gut microbiome during and after cancer treatment. This is now being tested in the setting of plasma cell myeloma, a bone marrow cancer, in which disturbance of the gut microbiome is thought to be associated with the development and progression of the cancer. Researchers at Memorial Sloan Kettering Cancer Center, led by Dr Urvi Shah, have begun a study using a whole food plant-based dietary intervention in people receiving treatment for myeloma. This is on the basis of prior data showing that healthier, plant-based dietary patterns were associated with higher levels of faecal butyrate, a SCFA, and longer remission in people with myeloma.

ALCOHOL AND CANCER: I come down hard on alcohol. There is no safe limit when it comes to cancer prevention and surviving well after a cancer diagnosis. Alcohol is classified as a group 1 carcinogen and is a direct cause of seven different cancer types. The paper highlighted demonstrates that in the US at least the message is not getting through to people with cancer. The study shows that alcohol consumption and risky drinking behaviours are common among cancer survivors, even among individuals receiving treatment. As health professionals, we need to do better to support patients, families and communities to reduce and eliminate alcohol consumption.

PLANT-BASED DIETS FOR PEOPLE LIVING WITH CANCER: There is now emerging data that a plant-based diet may be useful for addressing some of the common symptoms in people living with cancer report. For example, there are small studies reporting that a whole food plant-based diet may be useful for managing fatigue in people with lymphoma and breast cancer. In addition, a plant-based diet may also improve cognitive function in people with breast cancer and quality of life in people with prostate cancer. More studies are needed in people with established cancer and for those undergoing cancer treatment, however, there is plenty of supportive data on plant-based diets for prevention and management of other chronic conditions that affect people with cancer, such as cardiovascular disease and type 2 diabetes and may be useful in mitigating side-effects of cancer treatments. In addition, from the available data, albeit limited, there is evidence that a plant-based dietary pattern may improve overall survival following a diagnosis of cancer.

CANCER AND CHRONIC CONDITIONS: Not only do chronic conditions such as type 2 diabetes, cardiovascular disease and autoimmune conditions increase the risk of developing cancer but these chronic conditions are more common after a diagnosis of cancer. Healthy diet and lifestyle after a cancer diagnosis can significantly reduce the risk of cardiovascular disease and type 2 diabetes, with each incremental improvement in risk factors being of benefit. In addition, a healthy diet along side other healthy lifestyle behaviours, is important for reducing the increased risk of second cancers in people who have already had a first cancer.
If you have enjoyed this article, you can learn more on plant-based diets, chronic conditions, cancer and more at the VegMed conference in London on 9/10th September 2023. Hope to see you there.
Please follow my organisation ‘plant-based health professionals UK’ on Instagram @plantbasedhealthprofessionals and facebook. You can support our work by joining as a member or making a donation via the website.
