Review of the plant-based nutrition news November 2023
This month I highlight key evidence for shifting diets towards consuming more plants. The benefits include reduction in chronic diseases, increase in life expectancy, better cardiometabolic health and lower risk of cancer. Plant-based diets are appropriate for children and necessary to protect planetary health.

PREVENTION OF CHRONIC CONDITIONS: Unhealthy diets are the leading cause of chronic ill health and premature death. Yet there is consensus amongst health professionals and researchers on the key constituents of a healthy diet pattern. This is one that is high in plant foods and low in red/processed meat and ultra-processed foods and drinks. Based on this knowledge, various dietary scores have been created to assess diet quality in populations and correlate this with health outcomes.
This study evaluated the impact of 8 different dietary patterns using validated scoring systems amongst 205,852 women and men from the Nurses’ Health Study and Health Professionals Follow-up Study, followed for a median of 26 years. The impact of these dietary patterns on the risk of cardiovascular disease, type 2 diabetes and cancer was assessed. The healthful plant-based diet index was one of the 8 diet patterns assessed along-side Mediterranean and DASH diet scores and others. In addition, two mechanism-based dietary patterns were assessed: Empirical dietary index for hyperinsulinaemia and empirical dietary inflammation pattern.
In general, adherence to all the healthy diet patterns was associated with significant reductions in the risk of the chronic conditions assessed. The risk reductions seen were in the order of 10–40% with the greatest impact for the reduction in type 2 diabetes (up to 65%). The greatest reduction in risk was observed from low insulinaemic, low inflammatory, and diabetes risk-reducing diet patterns. However, adjusting for body mass index (BMI) attenuated some of the risk reduction.
Overall, the results suggest that the benefits of a healthy diet are due to their ability to prevent insulin resistance and reduce inflammation, key mechanims that drive the development of many of our common chronic conditions. In addition, maintaining a healthy body weight throughout life is important. We have clear evidence from prior data that a healthy plant-based diets, including vegetarian and vegan, are able to reduce the risk of insulin resistance, reduce inflammation, support a healthy body weight and are effective at reducing the risk of diabetes.

INCREASING LIFE EXPECTANCY: Despite knowing a lot about the key components of a healthy diet pattern and having evidence-based dietary guidance, the vast majority of people are not adhering to these guidelines. In the UK, less than 0.1% of the population meet the recommendation of our dietary guideline — The Eatwell Guide. This new paper uses a previously developed model for estimating the gain or loss in life expectancy in men and women aged 40–70 years following sustained dietary changes. The researchers used dietary data from 467,354 participants of the UK Biobank Study. The median dietary patterns in the UK were categorised as the intake level within the mid-quintile intake of each of the food groups.
The results showed that the longevity-associated dietary pattern had moderate intakes of whole grains, fruit, fish and white meat; a high intake of milk and dairy, vegetables, nuts and legumes; a relatively low intake of eggs, red meat and sugar-sweetened beverages; and a low intake of refined grains and processed meat. Some of the impact of these foods was attenuated when adjusting for body mass index. The unhealthy dietary pattern contained no or limited amounts of whole grains, vegetables, fruits, nuts, legumes, fish, milk and dairy, and white meat and substantial intakes of processed meat, eggs, refined grains and sugar-sweetened beverages. The strongest positive associations with mortality were for sugar-sweetened beverages and processed meat, while the strongest inverse associations with mortality were for whole grains, fruit and nuts.
The results showed that regardless of age, a shift towards a healthier diet pattern resulted in an increase in life expectancy. Shifting from the median UK diet to a healthy diet increased life expectancy by around 3 years for a 40-year-old and 1.7 years for a 70-year-old. Shifting from an unhealthy diet to a healthy diet increased life expectancy by 10 years in a 40-year-old and 5 years in a 70-year-old. The estimates were slightly lower after adjusting for energy intake and body mass index. Consuming less sugar-sweetened beverages and processed meats and eating more whole grains, fruits and nuts were estimated to result in the biggest improvements in life expectancy.
Prior studies have shown similar gains in life expectancy and importantly healthy life expectancy when shifting to a healthy diet pattern with benefits demonstrated regardless of age. For example, a similar analysis based on a US population showed significant gains in life expectancy when shifting from a typical Western diet to a healthy diet pattern regardless of age and with the greatest gains from consuming more whole grains, legumes and nuts. The Eat-Lancet commission estimated that by shifting to the plant-based health diet, this would save 11 million premature deaths that are currently caused by dietary risk factors. Another analysis from the UK Biobank cohort shows that greater adherence to the Eat Lancet reference diet resulted in a 9% reduction in risk of cancer and a 10% reduction in death from all causes.
The researchers from the current study call for policy changes that support people to access healthier foods, including health orientated food taxes and subsidises, improving the food environment and public sector catering and the need for multi-sector action including from the food industry.

IMPROVING CARDIOMETABOLIC HEALTH: There is little doubt that shifting away from consuming animals to eating a plant-based diet will improve our health.
This new study brings together data from 37 publications based on 24 prospective cohort studies with the aim of evaluating the available evidence for the substitution of any animal-based foods for plant-based foods on cardiometabolic health and all-cause mortality.
Overall the results showed that swapping any animal food for a plant-based food was beneficial for health, with risk reductions between 3–25%. The strongest associations were found for a reduction in cardiovascular disease when substituting processed meat for nuts, legumes and whole grains; substituting eggs for nuts; substituting butter for olive oil. For type 2 diabetes risk there were clear benefits for substituting red meat with whole grains, cereals and nuts; substituting poultry with whole grains; substituting eggs with nuts or whole grains. Reduction in death from all causes was found when substituting red meat for nuts and whole grains; processed meat with nuts and legumes; dairy with nuts; eggs with nuts and legumes. There was less clear evidence for substituting fish for plant-based foods.
It is notable that fairly small substitutions were shown to have significant benefits with portion sizes per day of 50g processed meat, 50g nuts, 50g legumes, 30g whole grains, one egg, 5g butter/olive oil contributing to positive or negative health impacts.
Overall, the results confirm prior data, and support the findings of numerous intervention studies that have shown improved health outcomes when shifting to a plant-based diet. The greatest gains for health are when meat is replaced by legumes, nuts and whole grains, but even replacing eggs and dairy is beneficial. There are so many reasons for these findings, including that plant foods are rich in fibre and other beneficial nutrients that reduce inflammation, support a healthier gut microbiome and regulate blood lipids, glucose and blood pressure more effectively. In contrast, these foods are low/absent in nutrients that harm health including saturated fat, haem iron and branched chain amino acids.
The data are clear, shifting away from animal-sources foods and prioritising plant-based foods is essential for maintaining health and well-being and has significant co-benefits for planetary health.

FIBRE INTAKE AND CANCER RISK REDUCTION: A plant-based diet is one of the key recommendations for preventing cancer and living well after a cancer diagnosis. One of the key anti-cancer components of a plant-based diet is fibre, a nutrient that most people do not consume enough of.
This paper analyses the impact of fibre intake on cancer risk, with a focus on different sources of fibre, in 364,856 participants from the UK Biobank study. During the 8.8 years of follow-up, 30,725 people were diagnosed with cancer. The results showed that people consuming the highest quintile of dietary fibre compared to the lowest quintile (<9.6 vs ≥19.1 g/day) had a 10% lower risk of cancer overall. The greatest reductions were observed for cervical, oesophageal, lung, bladder and kidney cancers. Fibre from cereal, fruit and vegetables had the greatest impact on risk reduction. The associations with colorectal cancer were not as large as expected, which may have been due to the fact that the highest quintile of fibre intake was relatively low >19.1g/day when in fact the ideal intake is >30g/day or more.
Fibre promotes health through increasing satiety and hence helping to maintain a healthy weight (important for cancer prevention). Foods high in fibre are also rich in health-promoting vitamins, minerals, antioxidant and anti-inflammatory compounds. Fibre is key to maintaining a healthy gut microbiome, which in turns supports a healthier immune system, glucose regulation and reduces inflammation. These mechanisms are all important for reducing cancer risk.

NOT ALL ULTRA-PROCESSED FOODS ARE CREATED EQUAL: There has been a lot of attention on ultra-processed foods (UPFs) recently, and rightly so. However, some of this attention is being used to create a negative narrative around vegan diets, suggesting that products frequently consumed by vegans fall into this UPF category. For example plant milks and plant-based meat alternatives are often deemed to be highly processed and hence considered by some to be unhealthy. This is then being used as an excuse to continue promoting the consumption of meat, milk and eggs as they are ‘natural’ and ‘unprocessed’.
This new analysis clearly shows that not all UPFs are created equal and thus highlights issues around the NOVA classification. This prospective cohort study included 266,666 participants (60% women) from the EPIC (European Prospective Investigation into Cancer and Nutrition) study. The median age at recruitment was 52 years and participants were followed for a median of 11.2 years. The mean consumption of UPFs (without alcoholic drinks) for men and women was 413 g/day and 326 g/day, respectively. This corresponded to a proportion of 34% kcal and 32% kcal of UPFs in the daily diet among men and women (much lower than the UK consumption where more than half of calories are from UPFs).
As expected, UPF consumption was associated with an increased risk of cardiometabolic conditions-cardiovascular disease and type 2 diabetes- and cancer. Each 260g/d increment in intake was associated with a 9% higher risk of these conditions (that is, of developing 2 of these diseases). Associations with higher BMI did explain some but not all of this increased risk. However, the increased risk was specifically associated with the consumption of artificially and sugar-sweetened beverages, animal-based products (including processed meats) and sauces, spreads and condiments. There was no increased risk of the cardiovascular disease, type 2 diabetes and cancer with consumption of other types of UFPs, such as breads and cereals, sweets and desserts, savoury snacks, plant-based alternatives, ready to eat/heat and mixed dishes. In fact the consumption of bread and cereals was inversely associated with these chronic conditions.
The results suggest that there may be non-nutritional reasons for the health harms associated with certain UPFs, including alteration of the food matrix, inclusion of certain food additives during processing (e.g., aspartame), and contaminants from packaging material (e.g., bisphenol A). These may affect endocrine pathways or the gut microbiome and contribute to subsequent disease risk. However, each product should be assessed on their own merit.

PLANT-BASED DIETS FOR CHILDREN AND ADOLESCENTS: This is a very useful study, similar to one published by the same authors on adults. The aim was to evaluate the nutrient intake and status of children and adolescents (2–18 years) consuming plant-based (i.e., vegetarian and vegan) diets compared to those of meat-eating children. A systematic literature review of studies published between 2000 and 2022 was conducted. Mean intake and status data of nutrients were calculated across studies and benchmarked to dietary reference values and cut-off values for nutrient deficiencies. A total of 30 studies were included (15 in children 2–5 years, 24 in children 6–12 years, and 11 in adolescents 13–18 years).
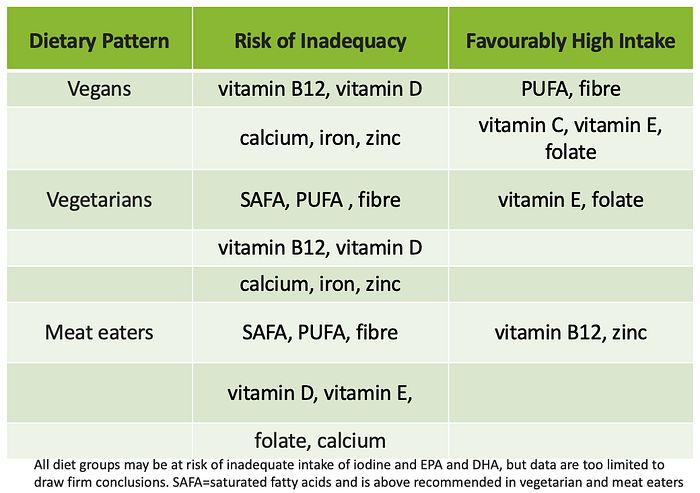
The results showed that in all diets there were risks of inadequate intakes of vitamin D and calcium. Regarding energy and protein intakes, most studies showed all diet patterns met recommended requirements. As expected, fibre intake was highest amongst vegans and insufficient in meat eaters. Saturated fatty acid intake was higher and PUFA (polyunsaturated fatty acid) lower than recommended in meat eaters. Insufficient and mixed data were present on intake of omega-3 fatty acids -EPA and DHA-and limited data are available for iodine intake. Iron intakes were deemed to be lower in those consuming meat-free diets due to the known lower bioavailability of iron from plant sources. Iron stores (ferritin levels) were lower in vegan and vegetarians, but this did not result in an increased risk of anaemia with no significant differences found in haemoglobin levels between diet groups. Similarly with zinc intake, bioavailability from plant sources is lower, but studies did not demonstrate deficiency in children consuming meat-free diets. Vitamin B12 needs to be supplemented in vegan diets.
Overall, the authors conclude that all three diet patterns could benefit from being optimised and that vegetarians and meat eaters could benefit from consuming more plant foods. Whereas for children on meat-free diets it is essential they consume a large variety of nutrient-dense plant foods (i.e., high in iron, zinc, iodine, calcium, and vitamins B12 and D) and/or foods, e.g., that are appropriately fortified with these micronutrients, e.g., dairy and meat alternatives. ‘Children on a plant-based diet as well as meat-eating children are at risk of inadequate nutrient intakes….. Increasing consumption of a variety of nutrient-rich plant foods, in combination with food fortification and possibly supplementation, can help children and adolescents have more sustainable diets that are healthier and meet all nutrient requirements’.
Check out this excellent factsheet on plant-based diets for children

DIET CHANGE NOT CLIMATE CHANGE: Two publications provide us with a warning that indicators of planetary health are way off course. The first by William Ripple et al ‘The 2023 state of the climate report: Entering uncharted territory’ and the second from the Lancet Countdown. They summarise the increasing and frequent impact of climate-related disasters such as flooding, extreme temperatures, wildfires and storms. The human health risks are the focus of this year’s Lancet countdown report. Phasing out fossil fuels and transitioning away from animal agriculture are highlighted as key actions required to avert disaster.
The Lancet report once again highlights that the current food system is not fit for purpose with 735 million people facing hunger and 3·1 billion people (42%) unable to afford a healthy diet. At the same time, 12.2. million deaths globally are attributable to dietary risk factors, namely, the insufficient consumption of fruits, vegetables, legumes, whole grains, nuts, and seeds, and an excess consumption of diary and red and processed meat. Additionally, the production of dairy, red and processed meat contribute to 57% of agricultural emissions whilst being responsible for 16% of all diet-related deaths (1·9 million). Very high HDI (Human Development Index) countries experienced the highest diet-related death rate; 2·4-times higher than the rate in low HDI countries. The very high HDI group also had the highest death rate related to excess dairy and red and processed meat consumption; 6·7-times higher than the average mortality for countries in other HDI groups. Animal agriculture is also a leading driver of biodiversity loss, land use changes and water, land and air pollution. Thus, the recommendations are clearly stated and require us to all transition to a ‘low carbon, plant-forward diet’. With less than a decade in which to make a difference, the window of opportunity is rapidly closing.
There are several useful sustainability toolkits for healthcare professionals that include guidance on plant-based diets. Examples include one from the Irish College of GPs and one for Canadian Family Doctors.
Please follow my organisation ‘plant-based health professionals UK’ on Instagram @plantbasedhealthprofessionals and facebook. You can support our work by joining as a member or making a donation via the website.
